These videos give an overview of the various Home and Community-Based Services (HCBS) available in Rhode Island for providers who want to learn how to start or operate an HCBS agency in the state. Each video explains the purpose of the service, provider requirements, licensing process, and how the program functions. Use these videos to better understand the responsibilities, standards, and steps involved in becoming or working with approved HCBS providers in Rhode Island. Explore each section to find the service that best matches your goals or area of interest.
Respite Care
RESPITE CARE SERVICES PROVIDER IN RHODE ISLAND
PROVIDING TEMPORARY RELIEF FOR FAMILY CAREGIVERS WHILE SUPPORTING INDIVIDUALS WITH COMPASSIONATE, DEPENDABLE CARE AT HOME OR IN THE COMMUNITY
Respite Care Services in Rhode Island are short-term, Medicaid-funded supports designed to provide relief to primary caregivers of individuals with disabilities, chronic illnesses, or age-related conditions. These services can be delivered in-home or in community-based settings to ensure the individual’s health and safety while the caregiver takes a break. Respite is authorized under Rhode Island’s Medicaid 1115 Waiver and various Long-Term Services and Supports (LTSS) programs, and can be arranged through managed care entities or self-direction.
1. GOVERNING AGENCIES
Agency: Rhode Island Executive Office of Health and Human Services (EOHHS)
Role: Administers Medicaid programs, including HCBS waivers that cover respite care services.
Agency: Rhode Island Department of Behavioral Healthcare, Developmental Disabilities & Hospitals (BHDDH)
Role: Oversees developmental disability programs and funds for respite under DD Waivers.
Agency: Centers for Medicare & Medicaid Services (CMS)**
Role: Provides federal oversight of Medicaid-funded respite services.
Agency: Rhode Island Department of Health (RIDOH)
Role: Licenses home care agencies providing in-home respite services, when required.
2. RESPITE CARE SERVICES OVERVIEW
Respite services provide temporary support to individuals with disabilities or significant care needs, allowing unpaid caregivers (e.g., family) to rest or attend to personal matters.
Approved providers may deliver:
In-Home Respite: Supervision, companionship, and assistance with ADLs in the individual's home.
Community-Based Respite: Care provided in a licensed respite facility, day program, or other approved setting.
Overnight Respite (optional): Extended relief care for several hours or days, often arranged in specialized settings.
Behavioral and Medical Support (as authorized): Assistance tailored to individuals with high support needs.
Documentation: Visit records, caregiver reports, and Medicaid-compliant billing forms.
3. LICENSING & PROVIDER APPROVAL REQUIREMENTS
Prerequisites:
Register your business with the Rhode Island Secretary of State.
Obtain an EIN and Type 2 NPI.
If providing in-home services: Apply for licensure as a Home Care Provider through RIDOH.
Enroll in Rhode Island Medicaid via the EOHHS provider portal.
Contract with BHDDH (for DD respite) or Medicaid managed care entities (e.g., Neighborhood Health Plan).
Maintain general liability and workers’ compensation insurance.
Develop a Respite Care Policy & Procedure Manual aligned with Medicaid and waiver requirements.
4. RHODE ISLAND PROVIDER ENROLLMENT PROCESS
Step 1: Establish your business entity and secure your EIN, NPI, and business insurance.
Step 2: If delivering home-based services, apply for RIDOH licensure as a home care agency.
Step 3: Enroll in the Medicaid system through the EOHHS provider portal.
Step 4: Contract with BHDDH or Medicaid MCOs, depending on the population served.
Step 5: Submit staff credentials, service protocols, and your policy manual for approval.
Step 6: Begin receiving respite service authorizations and caregiver referrals.
5. REQUIRED DOCUMENTATION
Articles of Incorporation and business registration
EIN and NPI confirmations
RIDOH Home Care License (if applicable)
Insurance certificates (general, workers’ comp)
Respite Care Services Policy & Procedure Manual including:
Caregiver intake and scheduling procedures
ADL task documentation and daily shift notes
Emergency and critical incident protocols
Participant rights and safety policies
HIPAA compliance and abuse prevention guidelines
Respite authorization tracking and Medicaid billing forms
6. STAFFING REQUIREMENTS
Role: Respite Aide / Direct Support Professional (DSP)
Requirements: CPR/First Aid certified; background check; relevant training in personal care and safety.
Role: Program Supervisor (RN or Human Services Professional)
Requirements: Oversees care planning and staff compliance; licensed professionals may be required for medically fragile participants.
All staff must complete:
HIPAA and participant rights training
Abuse and neglect prevention education
ADL assistance and documentation training
Emergency procedures and incident response
Annual skills assessments and competency checks
7. MEDICAID WAIVER PROGRAMS
Respite care is authorized through:
Global Consumer Choice Compact 1115 Waiver (RI Medicaid): Covers in-home and community-based respite as part of HCBS.
BHDDH DD Waivers: Includes respite for individuals with developmental disabilities living at home with family caregivers.
Katie Beckett Program: For medically eligible children with complex needs.
Self-Directed Services (through fiscal intermediaries): Allows families to hire qualified respite workers directly.
8. TIMELINE TO LAUNCH
Phase: Business Formation & Policy Manual Development
Timeline: 1–2 months
Phase: RIDOH Licensure & Medicaid Enrollment
Timeline: 2–3 months
Phase: Staff Hiring, Training & Credentialing
Timeline: 30–60 days
Phase: Readiness Review & Referral Activation
Timeline: Begins after contracting and Medicaid authorization
9. CONTACT INFORMATION
Rhode Island Executive Office of Health and Human Services (EOHHS)
Website: https://eohhs.ri.gov
Rhode Island Medicaid Provider Portal
Website: https://www.riproviderportal.org
Department of Behavioral Healthcare, Developmental Disabilities & Hospitals (BHDDH)
Website: https://bhddh.ri.gov
Rhode Island Department of Health – Home Care Licensure
Website: https://health.ri.gov/licenses/detail.php?id=282
Centers for Medicare & Medicaid Services (CMS)
Website: https://www.cms.gov
WAIVER CONSULTING GROUP’S START-UP ASSISTANCE SERVICE — RHODE ISLAND RESPITE CARE PROVIDER
WCG supports Rhode Island agencies in launching licensed, waiver-approved respite care programs that meet Medicaid standards and family caregiver needs.
Scope of Work:
Business registration, RIDOH licensure, and Medicaid enrollment
Respite Care Policy & Procedure Manual tailored to in-home and facility-based care
Staff onboarding, documentation, and emergency response protocols
ADL task logs, caregiver intake forms, and shift notes
Contracts with BHDDH, Medicaid MCOs, and self-direction support
Audit-readiness templates and compliance checklists

Residential Care
RESIDENTIAL CARE SERVICES PROVIDER IN RHODE ISLAND
SUPPORTING COMMUNITY-BASED LIVING WITH 24/7 CARE AND INDEPENDENCE FOR INDIVIDUALS WITH DISABILITIES OR COMPLEX NEEDS
Residential Care Services in Rhode Island provide long-term, round-the-clock support to individuals who require supervised living arrangements due to developmental disabilities, behavioral health needs, or complex medical conditions. These services are primarily funded under the state’s Medicaid 1115 Global Waiver and managed by the Department of Behavioral Healthcare, Developmental Disabilities & Hospitals (BHDDH) and the Executive Office of Health and Human Services (EOHHS). Residential options range from group homes to shared living environments and staffed apartments.
1. GOVERNING AGENCIES
Agency: Rhode Island Executive Office of Health and Human Services (EOHHS)
Role: Oversees Medicaid funding, provider enrollment, and residential program compliance under the 1115 waiver.
Agency: Department of Behavioral Healthcare, Developmental Disabilities & Hospitals (BHDDH)
Role: Licenses and monitors residential service providers for individuals with IDD.
Agency: Rhode Island Department of Health (RIDOH)**
Role: Regulates facility safety, infection control, and clinical oversight if health-related services are provided.
Agency: Centers for Medicare & Medicaid Services (CMS)**
Role: Ensures federal HCBS compliance and residential setting standards.
2. RESIDENTIAL CARE SERVICES OVERVIEW
Residential care provides a structured, home-like environment with individualized services that support personal development, health, and community involvement.
Approved providers may deliver:
24-Hour Supervision & Support: Trained staff present at all times for assistance and safety.
Personal Care & ADL Support: Bathing, dressing, grooming, toileting, and mobility assistance.
Medication Administration: RN oversight or delegated staff for medication delivery.
Behavioral Support Services: Implementation of behavior plans and mental health support.
Life Skills Development: Cooking, laundry, cleaning, and self-advocacy coaching.
Community Integration: Day programming, volunteer work, outings, and social skill-building.
Individualized Service Plan (ISP) Implementation: Tailored goals and progress documentation.
Transportation Coordination: To appointments, work, or social events.
3. LICENSING & PROVIDER APPROVAL REQUIREMENTS
Prerequisites:
Register your business entity with the Rhode Island Secretary of State.
Obtain an EIN and Type 2 NPI.
Submit a residential services provider application to BHDDH.
Comply with RIDOH health and safety regulations for facilities (if applicable).
Meet HCBS Final Rule standards for person-centered, integrated residential settings.
Develop a Residential Services Policy & Procedure Manual that includes safety, staffing, ISP implementation, and documentation protocols.
4. RHODE ISLAND PROVIDER ENROLLMENT PROCESS
Step 1: Form a legal entity and acquire EIN, NPI, and required insurance.
Step 2: Apply for provider approval with BHDDH for residential supports.
Step 3: Prepare a staffing plan, physical site review, and policy manual submission.
Step 4: Enroll with Medicaid through the RI provider portal and submit credentials.
Step 5: Upon approval, receive participant referrals and begin ISP-based service delivery.
5. REQUIRED DOCUMENTATION
Articles of Incorporation and business registration
EIN and NPI confirmations
Proof of Medicaid and BHDDH enrollment
Property compliance (zoning, fire safety, occupancy limits)
Insurance certificates (liability, workers’ comp, property, vehicle)
Residential Services Policy & Procedure Manual including:
Supervision and staffing ratios
Emergency procedures and incident reporting
ISP implementation and progress monitoring
Medication administration and health oversight
Participant rights, privacy, and abuse prevention
House rules and visitor policies
6. STAFFING REQUIREMENTS
Role: Direct Support Professional (DSP)
Requirements: CPR/First Aid, background check, abuse prevention training, person-centered service experience.
Role: House Manager or Residential Supervisor
Requirements: Staff scheduling, training oversight, ISP coordination, and home operations.
Role: Registered Nurse (if required)
Requirements: Supports medication oversight, health monitoring, and documentation reviews.
Role: Behavior Specialist (if authorized)
Requirements: Develops and monitors behavioral support plans.
All staff must complete:
HIPAA and mandatory reporting training
ISP documentation and outcome tracking
Emergency preparedness and safety drills
Annual skills review and professional development
Community inclusion and client rights education
7. MEDICAID WAIVER PROGRAMS
Residential Care Services are funded through:
BHDDH IDD Waivers (Community Living Arrangement): Primary source for residential group home funding.
Shared Living Arrangement Waiver: Family-style living with stipends and oversight.
1115 Global Waiver (HCBS): Allows innovative models for residential support.
Self-Directed Waivers: Participants may choose residential services from approved providers.
8. TIMELINE TO LAUNCH
Phase: Business Formation & Policy Manual Creation
Timeline: 1–2 months
Phase: BHDDH Application & Medicaid Enrollment
Timeline: 2–3 months
Phase: Property Setup, Staff Hiring & Training
Timeline: 30–60 days
Phase: Participant Referral & Service Start
Timeline: Begins after enrollment and successful readiness review
9. CONTACT INFORMATION
Rhode Island Executive Office of Health and Human Services (EOHHS)
Website: https://eohhs.ri.gov
Department of Behavioral Healthcare, Developmental Disabilities & Hospitals (BHDDH)
Website: https://bhddh.ri.gov
Rhode Island Department of Health (RIDOH)
Website: https://health.ri.gov
Rhode Island Medicaid Provider Portal
Website: https://www.riproviderportal.org
Centers for Medicare & Medicaid Services (CMS)
Website: https://www.cms.gov
WAIVER CONSULTING GROUP’S START-UP ASSISTANCE SERVICE — RHODE ISLAND RESIDENTIAL CARE PROVIDER
WCG supports residential providers in Rhode Island with launching HCBS-compliant housing programs tailored to individuals with IDD and complex needs.
Scope of Work:
BHDDH provider application and Medicaid enrollment
Residential care-focused Policy & Procedure Manual
Staff credentialing tools and 24/7 scheduling templates
ISP progress forms and service documentation logs
House rules, incident tracking, and emergency response guides
Licensing prep and fire inspection readiness checklists

Supported Employment
SUPPORTED EMPLOYMENT SERVICES PROVIDER IN RHODE ISLAND
EMPOWERING INDIVIDUALS WITH DISABILITIES TO ACHIEVE MEANINGFUL WORK AND INDEPENDENCE THROUGH CUSTOMIZED EMPLOYMENT SUPPORTS
Supported Employment Services in Rhode Island provide individualized, ongoing supports to help people with intellectual and developmental disabilities (IDD) prepare for, obtain, and maintain paid employment in integrated community settings. These Medicaid-funded services are authorized under Rhode Island’s Home and Community-Based Services (HCBS) 1115 Waiver and are managed by the Department of Behavioral Healthcare, Developmental Disabilities & Hospitals (BHDDH) in partnership with the Executive Office of Health and Human Services (EOHHS).
1. GOVERNING AGENCIES
Agency: Rhode Island Executive Office of Health and Human Services (EOHHS)
Role: Oversees Medicaid waiver structure and provider enrollment for employment supports.
Agency: Department of Behavioral Healthcare, Developmental Disabilities & Hospitals (BHDDH)
Role: Authorizes supported employment services for participants with IDD and ensures compliance with Employment First goals.
Agency: Office of Rehabilitation Services (ORS)
Role: May provide pre-employment services and funding coordination with Medicaid.
Agency: Centers for Medicare & Medicaid Services (CMS)
Role: Ensures HCBS employment services meet federal guidelines under the Final Settings Rule.
2. SUPPORTED EMPLOYMENT SERVICES OVERVIEW
These services are designed to help individuals with disabilities find and succeed in competitive, integrated employment based on their strengths, preferences, and career goals.
Approved providers may deliver:
Career Planning & Discovery: Person-centered assessments to identify interests and work preferences.
Job Development: Resume preparation, job searches, application assistance, and employer outreach.
Job Coaching: On-the-job support and skill-building to promote independence.
Workplace Accommodations: Coordination with employers to ensure accessible and supportive environments.
Follow-Along Support: Ongoing check-ins and adjustments to maintain employment over time.
Self-Employment Support (if authorized): Business planning and support for microenterprises.
Documentation: Individualized Employment Plans (IEPs), progress notes, and outcome reporting.
3. LICENSING & PROVIDER APPROVAL REQUIREMENTS
Prerequisites:
Register your business with the Rhode Island Secretary of State.
Obtain an EIN and Type 2 NPI.
Enroll with BHDDH as an IDD Employment Services Provider.
Submit staffing plan, policy manual, and employment support model.
Contract with Medicaid through the RI provider portal.
Maintain general liability and workers’ compensation insurance.
Develop a Supported Employment Services Policy & Procedure Manual that outlines career planning, service delivery, and documentation standards.
4. RHODE ISLAND PROVIDER ENROLLMENT PROCESS
Step 1: Form legal entity and obtain EIN, NPI, and insurance.
Step 2: Apply to BHDDH for employment provider approval.
Step 3: Submit program design, service locations, and staff qualifications.
Step 4: Enroll with RI Medicaid and secure service authorizations.
Step 5: Begin receiving participant referrals and provide job support services.
5. REQUIRED DOCUMENTATION
Articles of Incorporation and registration
EIN and NPI confirmation
Insurance certificates
BHDDH provider approval confirmation
Supported Employment Services Policy & Procedure Manual including:
Career discovery, vocational assessments, and employer engagement plans
Job coaching logs and follow-up documentation
Participant rights, safety protocols, and privacy policies
Crisis prevention and workplace incident response plans
Medicaid billing forms and outcome reporting templates
Annual satisfaction surveys and quality assurance procedures
6. STAFFING REQUIREMENTS
Role: Employment Specialist / Job Coach
Requirements: Background check, experience with vocational support, CPR/First Aid, and BHDDH-approved employment services training.
Role: Employment Services Supervisor
Requirements: Knowledge of ADA, workforce development, Medicaid service documentation, and staff management.
All staff must complete:
HCBS Settings Rule and Employment First training
Person-centered planning and ISP implementation
Community safety, transportation protocols, and workplace etiquette training
Documentation and HIPAA compliance
Crisis de-escalation and professional boundaries education
7. MEDICAID WAIVER PROGRAMS
Supported Employment Services are authorized under:
BHDDH IDD Waivers (Community Living Arrangement, Shared Living, Self-Directed): Core waiver funding for employment supports.
1115 Global Waiver: Allows integrated funding models for employment-first initiatives.
Self-Directed Supports: Individuals may select and contract with approved employment providers.
ORS Partnership Funding: May be braided with Medicaid supports for pre-vocational and initial job placement phases.
8. TIMELINE TO LAUNCH
Phase: Business Formation & Manual Development
Timeline: 1–2 months
Phase: BHDDH Employment Services Application
Timeline: 1–2 months
Phase: Medicaid Enrollment & Staff Training
Timeline: 30–60 days
Phase: Participant Referrals & Job Matching
Timeline: Begins after approval and ISP authorization
9. CONTACT INFORMATION
Rhode Island Executive Office of Health and Human Services (EOHHS)
Website: https://eohhs.ri.gov
Department of Behavioral Healthcare, Developmental Disabilities & Hospitals (BHDDH)
Website: https://bhddh.ri.gov
Rhode Island Medicaid Provider Portal
Website: https://www.riproviderportal.org
Office of Rehabilitation Services (ORS)
Website: https://ors.ri.gov
Centers for Medicare & Medicaid Services (CMS)
Website: https://www.cms.gov
WAIVER CONSULTING GROUP’S START-UP ASSISTANCE SERVICE — RHODE ISLAND SUPPORTED EMPLOYMENT PROVIDER
WCG helps employment providers design and implement mission-driven, compliance-ready services that connect individuals with IDD to meaningful jobs.
Scope of Work:
BHDDH application and Medicaid enrollment
Supported Employment Policy & Procedure Manual
Staff credentialing checklists and ISP-aligned documentation
Employer engagement templates and safety protocols
Billing tools and job coaching logs
Employment outcome tracking and quarterly report templates

Personal Care
PERSONAL CARE SERVICES PROVIDER IN RHODE ISLAND
SUPPORTING INDEPENDENCE, DIGNITY, AND DAILY FUNCTIONING FOR ELDERS AND INDIVIDUALS WITH DISABILITIES THROUGH COMPASSIONATE IN-HOME SUPPORT
Personal Care Services (PCS) in Rhode Island are non-medical supports funded by Medicaid to assist individuals who need help with activities of daily living (ADLs) such as bathing, dressing, mobility, and meal preparation. These services enable individuals to remain safely in their homes and avoid institutional care. PCS are offered through Rhode Island Medicaid’s Long-Term Services and Supports (LTSS) system and may be authorized under State Plan benefits or the Home and Community-Based Services (HCBS) Waiver programs.
1. GOVERNING AGENCIES
Agency: Rhode Island Executive Office of Health and Human Services (EOHHS)
Role: Administers Medicaid programs, including PCS and LTSS authorizations.
Agency: Office of Healthy Aging (OHA)
Role: Manages the state’s Aging and Disability Resource Center (The POINT) and may refer individuals to PCS providers.
Agency: Centers for Medicare & Medicaid Services (CMS)**
Role: Regulates Medicaid LTSS programs under federal HCBS guidelines.
Agency: Rhode Island Department of Health (RIDOH)
Role: Licenses home care agencies and monitors health and safety standards for in-home services.
2. PERSONAL CARE SERVICES OVERVIEW
PCS support individuals who are medically stable but need daily assistance to maintain independence at home.
Approved providers may deliver:
Assistance with ADLs: Bathing, grooming, dressing, toileting, eating, and mobility.
Meal Preparation & Light Housekeeping: Cooking meals, washing dishes, laundry, and tidying the home.
Supervision & Safety Monitoring: Ensuring a safe environment for individuals with memory loss or fall risks.
Medication Reminders (non-clinical): Encouraging adherence to prescribed medications.
Accompaniment to Appointments: Escorting individuals to local appointments or errands (non-medical transport only).
Care Documentation: Visit notes, ADL task checklists, incident reporting, and service verification.
3. LICENSING & PROVIDER APPROVAL REQUIREMENTS
Prerequisites:
Register your business entity with the Rhode Island Secretary of State.
Obtain a Federal EIN and Type 2 NPI.
Apply for licensure as a Home Care Provider Agency through RIDOH.
Enroll as a Medicaid PCS provider via the Rhode Island Medicaid portal.
Maintain general liability and workers’ compensation insurance.
Develop a Personal Care Services Policy & Procedure Manual aligned with RIDOH and Medicaid requirements.
4. RHODE ISLAND PROVIDER ENROLLMENT PROCESS
Step 1: Form your business entity and obtain EIN and NPI.
Step 2: Apply for Home Care Agency licensure through RIDOH.
Step 3: Enroll in the Rhode Island Medicaid program as a PCS provider.
Step 4: Submit all required documentation, including policy manual, staff credentials, and insurance.
Step 5: Receive approval and begin accepting service authorizations and referrals.
5. REQUIRED DOCUMENTATION
Articles of Incorporation and business registration
EIN and NPI confirmation
RIDOH Home Care license
Insurance certificates (general, workers’ comp)
Personal Care Services Policy & Procedure Manual including:
ADL task procedures and client intake process
Emergency protocols and incident response
Participant rights and consent forms
Daily visit note and billing templates
Staff training, supervision, and documentation standards
HIPAA compliance and abuse prevention policies
6. STAFFING REQUIREMENTS
Role: Personal Care Aide / Homemaker
Requirements: Completion of PCA training (per RIDOH-approved curriculum), background checks, CPR/First Aid preferred.
Role: Registered Nurse (Supervisor)
Requirements: Active RI license; provides initial assessments, oversees care plans, and trains direct care staff.
Role: Scheduler / Program Coordinator
Requirements: Coordinates caregiver assignments, documentation collection, and compliance.
All staff must complete:
HIPAA and confidentiality training
Abuse recognition and mandatory reporting
Documentation and billing training
Annual in-service training (minimum hours required by RIDOH)
7. MEDICAID WAIVER PROGRAMS
PCS are reimbursed under the following programs:
Rhode Island Medicaid State Plan PCS Benefit: For eligible individuals requiring ADL assistance.
Global Consumer Choice Compact Waiver (1115 Waiver): Covers PCS and other HCBS under integrated managed care.
PACE RI & Medicaid Managed LTSS Plans: Provide PCS through contracted agencies.
Temporary Disability Programs (State-funded): May offer PCS for limited durations.
8. TIMELINE TO LAUNCH
Phase: Business Registration & Policy Manual Development
Timeline: 1–2 months
Phase: RIDOH Licensure & Medicaid Enrollment
Timeline: 2–3 months
Phase: Staff Hiring, Credentialing & Training
Timeline: 30–60 days
Phase: Referral Activation & Service Launch
Timeline: Begins upon approval by Medicaid and RIDOH
9. CONTACT INFORMATION
Rhode Island Executive Office of Health and Human Services (EOHHS)
Website: https://eohhs.ri.gov
Rhode Island Medicaid Provider Portal
Website: https://www.riproviderportal.org
Rhode Island Department of Health (RIDOH) – Home Care Licensing
Website: https://health.ri.gov/licenses/detail.php?id=282
Office of Healthy Aging (The POINT)
Website: https://oha.ri.gov
Centers for Medicare & Medicaid Services (CMS)
Website: https://www.cms.gov
WAIVER CONSULTING GROUP’S START-UP ASSISTANCE SERVICE — RHODE ISLAND PERSONAL CARE SERVICES PROVIDER
WCG supports providers in Rhode Island in launching compliant, compassionate Personal Care Services to meet growing LTSS needs.
Scope of Work:
Business registration, RIDOH licensure, and Medicaid enrollment
PCS Policy & Procedure Manual tailored to Rhode Island regulations
Staff credentialing tools and training logs
ADL task checklist templates and documentation guides
Referral strategies and intake coordination templates
Billing forms and audit readiness support

Adaptive Equipment
ADAPTIVE EQUIPMENT SERVICES PROVIDER IN RHODE ISLAND
ENHANCING INDEPENDENCE AND SAFETY THROUGH CUSTOMIZED EQUIPMENT SOLUTIONS FOR INDIVIDUALS WITH DISABILITIES AND FUNCTIONAL LIMITATIONS
Adaptive Equipment Services in Rhode Island are Medicaid-funded supports that help individuals obtain, maintain, and use devices that promote greater independence at home and in the community. These services are primarily funded through the state’s Medicaid 1115 Global Waiver and Developmental Disabilities (DD) Waivers. Adaptive equipment may include mobility aids, communication devices, self-care tools, and home accessibility supports.
1. GOVERNING AGENCIES
Agency: Rhode Island Executive Office of Health and Human Services (EOHHS)
Role: Oversees Medicaid authorization and reimbursement for adaptive equipment and assistive technology.
Agency: Department of Behavioral Healthcare, Developmental Disabilities & Hospitals (BHDDH)
Role: Authorizes and monitors equipment services under DD Waivers for individuals with disabilities.
Agency: Centers for Medicare & Medicaid Services (CMS)**
Role: Provides federal guidelines for Medicaid-funded durable medical equipment and HCBS settings.
Agency: Rhode Island Department of Health (RIDOH)**
Role: May regulate provider facilities or personnel if clinical assessments or medical customization is involved.
2. ADAPTIVE EQUIPMENT SERVICES OVERVIEW
These services ensure individuals with disabilities have access to equipment that helps them perform daily activities, communicate, and remain safe in their environment.
Approved providers may deliver:
Assessment & Recommendation: Evaluation of functional needs by therapists or specialists.
Procurement & Customization: Ordering and fitting of adaptive devices (e.g., walkers, communication aids, shower chairs).
Training & Instruction: Teaching participants and caregivers how to safely use equipment.
Maintenance & Repairs: Fixing or replacing equipment to ensure continued usability.
Documentation & Compliance: Recording needs, service delivery, and Medicaid billing forms.
3. LICENSING & PROVIDER APPROVAL REQUIREMENTS
Prerequisites:
Register your business with the Rhode Island Secretary of State.
Obtain EIN and Type 2 NPI.
Enroll as a Medicaid provider under adaptive equipment/DME codes or HCBS waiver support services.
Hire or contract with licensed occupational or physical therapists for assessments, as needed.
Maintain product liability and general business insurance.
Develop an Adaptive Equipment Services Policy & Procedure Manual covering safety, training, and documentation.
4. RHODE ISLAND PROVIDER ENROLLMENT PROCESS
Step 1: Register your business, secure EIN, NPI, and insurance.
Step 2: Apply to EOHHS for enrollment as a Medicaid HCBS provider or DME vendor.
Step 3: If servicing individuals with IDD, submit a provider application to BHDDH.
Step 4: Submit your policy manual, staffing plan, and product sourcing documentation.
Step 5: Begin receiving service authorizations and participant referrals.
5. REQUIRED DOCUMENTATION
Articles of Incorporation and state business registration
EIN and NPI confirmation
Medicaid enrollment acceptance
Therapist licenses or consultant contracts
Insurance coverage (product liability, general, workers' comp)
Adaptive Equipment Services Policy & Procedure Manual including:
Evaluation and recommendation process
Equipment training and caregiver instruction procedures
Safety protocols and maintenance schedules
Documentation and billing templates
Participant rights and consent forms
Repair/replacement workflows and Medicaid compliance
6. STAFFING REQUIREMENTS
Role: Occupational Therapist (OT) or Physical Therapist (PT)
Requirements: RI licensure, Medicaid credentials, experience in adaptive equipment assessment.
Role: Equipment Technician / Installer
Requirements: Knowledge of mobility/accessibility devices, safety training, background check.
Role: Program Coordinator
Requirements: Manages referrals, Medicaid authorizations, and participant service documentation.
All staff must complete:
HIPAA and participant rights training
Equipment use, safety, and troubleshooting instruction
Abuse prevention and incident reporting
Documentation and Medicaid billing training
Cultural sensitivity and family engagement education
7. MEDICAID WAIVER PROGRAMS
Adaptive Equipment Services are available through:
BHDDH DD Waivers (e.g., Community Living, Shared Living): Covers equipment not otherwise funded by Medicare/insurance.
1115 Global Waiver (HCBS): Authorizes adaptive devices for participants in community-based care.
Katie Beckett/TEFRA Program: Pediatric participants may receive customized equipment.
State Plan DME Coverage (when applicable): May coordinate with waiver services to avoid duplication.
8. TIMELINE TO LAUNCH
Phase: Business Formation & Manual Creation
Timeline: 1–2 months
Phase: Medicaid Enrollment & Staff Contracting
Timeline: 2–3 months
Phase: Vendor Sourcing & Referral Agreements
Timeline: 30–60 days
Phase: Participant Service Initiation
Timeline: Begins upon authorization and care plan approval
9. CONTACT INFORMATION
Rhode Island Executive Office of Health and Human Services (EOHHS)
Website: https://eohhs.ri.gov
Rhode Island Medicaid Provider Portal
Website: https://www.riproviderportal.org
Department of Behavioral Healthcare, Developmental Disabilities & Hospitals (BHDDH)
Website: https://bhddh.ri.gov
Rhode Island Department of Health (RIDOH)
Website: https://health.ri.gov
Centers for Medicare & Medicaid Services (CMS)
Website: https://www.cms.gov
WAIVER CONSULTING GROUP’S START-UP ASSISTANCE SERVICE — RHODE ISLAND ADAPTIVE EQUIPMENT PROVIDER
WCG supports providers launching adaptive equipment services that meet the specialized mobility and communication needs of Medicaid-eligible individuals in Rhode Island.
Scope of Work:
Medicaid and BHDDH enrollment guidance
Therapist contracting and licensure verification tools
Adaptive Equipment Policy & Procedure Manual development
Consent forms, training logs, and installation protocols
Repair tracking sheets and billing documentation templates
Vendor sourcing strategies and product liability guidance

Day Habilitation
DAY HABILITATION SERVICES PROVIDER IN RHODE ISLAND
FOSTERING SKILL DEVELOPMENT, SOCIAL PARTICIPATION, AND COMMUNITY ENGAGEMENT FOR INDIVIDUALS WITH DISABILITIES IN SUPPORTIVE DAY SETTINGS
Day Habilitation Services in Rhode Island are Medicaid-funded supports designed to promote the acquisition, retention, and improvement of self-help, socialization, and adaptive skills in individuals with intellectual and developmental disabilities (IDD). These services are delivered in non-residential, structured settings and aim to increase independence, communication, and participation in community life. Day habilitation is funded under Rhode Island’s Home and Community-Based Services (HCBS) 1115 Waiver and authorized through the Department of Behavioral Healthcare, Developmental Disabilities & Hospitals (BHDDH).
1. GOVERNING AGENCIES
Agency: Rhode Island Executive Office of Health and Human Services (EOHHS)
Role: Manages Medicaid funding, oversees the state’s 1115 Waiver, and approves provider enrollment.
Agency: Department of Behavioral Healthcare, Developmental Disabilities & Hospitals (BHDDH)
Role: Licenses and monitors day habilitation providers; oversees person-centered planning and service delivery for individuals with IDD.
Agency: Centers for Medicare & Medicaid Services (CMS)**
Role: Provides federal oversight and regulatory standards for HCBS-funded day habilitation services.
Agency: Rhode Island Department of Health (RIDOH)**
Role: May regulate facilities for safety compliance depending on the level of care offered onsite.
2. DAY HABILITATION SERVICES OVERVIEW
These services support individuals who require assistance with life skills development in a structured, community-based environment.
Approved providers may deliver:
Life Skills Training: Cooking, hygiene, communication, budgeting, and using public transportation.
Pre-Vocational Support: Workplace behavior, task completion, and job-readiness exercises.
Community Integration Activities: Outings, volunteering, and local engagement to build social skills.
Health and Wellness Programming: Basic physical activity, nutrition education, and wellness routines.
Peer Interaction: Group activities that enhance social participation and reduce isolation.
Service Documentation: Individualized service plans (ISPs), daily logs, progress reports, and billing records.
3. LICENSING & PROVIDER APPROVAL REQUIREMENTS
Prerequisites:
Register your business entity with the Rhode Island Secretary of State.
Obtain an EIN and Type 2 NPI.
Submit a provider application to BHDDH to operate as a day habilitation program.
If operating a physical site, ensure zoning compliance and RIDOH safety inspections as needed.
Maintain general liability, workers’ comp, and vehicle insurance (if transportation is offered).
Develop a Day Habilitation Services Policy & Procedure Manual in line with BHDDH standards.
4. RHODE ISLAND PROVIDER ENROLLMENT PROCESS
Step 1: Form your business and obtain EIN, NPI, and applicable insurance.
Step 2: Apply to become a BHDDH-approved DD services provider.
Step 3: Submit your program structure, facility information, staffing plan, and policies for review.
Step 4: Enroll as a Medicaid HCBS provider under the RI EOHHS provider portal.
Step 5: Complete service readiness reviews and begin receiving individual authorizations.
5. REQUIRED DOCUMENTATION
Articles of Incorporation and state registration
EIN and NPI confirmations
Insurance certificates (liability, workers’ comp, facility)
BHDDH provider approval letter
Day Habilitation Policy & Procedure Manual including:
Individualized support planning and goal tracking
Community integration and daily activity schedule
Participant rights, dignity, and safety policies
Incident reporting, abuse prevention, and emergency response
Staffing ratios, supervision, and ongoing staff development
Medicaid billing templates and ISP documentation procedures
6. STAFFING REQUIREMENTS
Role: Day Habilitation Specialist / Direct Support Professional (DSP)
Requirements: Experience supporting individuals with IDD; background check; CPR/First Aid; BHDDH-approved training.
Role: Program Manager / Supervisor
Requirements: Experience in disability services, staff management, and compliance; may be required to hold a relevant degree.
Role: Community Integration Coordinator (optional)
Requirements: Coordinates volunteer sites, community partnerships, and activity calendars.
All staff must complete:
Person-centered planning and ISP documentation training
Abuse, neglect, and mandatory reporting education
HIPAA and participant confidentiality protocols
Transportation safety (if applicable) and behavior management training
Annual professional development hours (per BHDDH guidelines)
7. MEDICAID WAIVER PROGRAMS
Day Habilitation Services are authorized through:
BHDDH DD Waivers (Community Living Arrangement, Shared Living, Self-Directed): Primary source of habilitation funding.
1115 Global Waiver (HCBS): Covers habilitation services for Medicaid-eligible individuals with IDD.
Self-Directed HCBS Waivers: Participants may choose habilitation services from qualified provider agencies.
Transition-Aged Youth Waivers (if applicable): Supports 18–21-year-olds exiting school-based services.
8. TIMELINE TO LAUNCH
Phase: Business Formation & Policy Manual Development
Timeline: 1–2 months
Phase: BHDDH Provider Approval & Medicaid Enrollment
Timeline: 2–3 months
Phase: Facility Setup, Staff Hiring & Training
Timeline: 30–60 days
Phase: Service Activation & ISP Authorizations
Timeline: Begins once participants are referred by BHDDH or self-directing case managers
9. CONTACT INFORMATION
Rhode Island Executive Office of Health and Human Services (EOHHS)
Website: https://eohhs.ri.gov
Rhode Island Medicaid Provider Portal
Website: https://www.riproviderportal.org
Department of Behavioral Healthcare, Developmental Disabilities & Hospitals (BHDDH)
Website: https://bhddh.ri.gov
Rhode Island Department of Health (RIDOH)
Website: https://health.ri.gov
Centers for Medicare & Medicaid Services (CMS)
Website: https://www.cms.gov
WAIVER CONSULTING GROUP’S START-UP ASSISTANCE SERVICE — RHODE ISLAND DAY HABILITATION PROVIDER
WCG helps providers in Rhode Island design and launch engaging, Medicaid-compliant day programs that empower individuals with IDD to thrive in community settings.
Scope of Work:
BHDDH provider application and Medicaid enrollment
Customized Day Habilitation Policy & Procedure Manual
Facility layout planning and activity schedule templates
ISP tracking sheets and participant goal progress tools
Staff training logs and abuse prevention documentation
Community integration activity planning and partner outreach tools

Skilled Nursing
SKILLED NURSING SERVICES PROVIDER IN PENNSYLVANIA
DELIVERING MEDICALLY NECESSARY CARE AT HOME TO PROMOTE HEALTH, RECOVERY, AND INDEPENDENCE
Skilled Nursing Services in Pennsylvania are Medicaid-funded, medically necessary services delivered by licensed nurses to individuals with complex health needs. These services are designed to prevent or delay institutionalization by providing clinical interventions in the individual’s home or community setting. Skilled nursing is covered under the Pennsylvania Medicaid State Plan, Home and Community-Based Services (HCBS) waivers, and Community HealthChoices (CHC) Managed Care Organizations (MCOs).
1. GOVERNING AGENCIES
Agency: Pennsylvania Department of Health (DOH) – Division of Home Health
Role: Licenses home health agencies that deliver skilled nursing care.
Agency: Pennsylvania Department of Human Services (DHS) – Office of Long-Term Living (OLTL)
Role: Oversees HCBS waiver programs that fund skilled nursing for aging and physically disabled populations.
Agency: Community HealthChoices (CHC) MCOs
Role: Authorize and reimburse for skilled nursing under managed Medicaid.
Agency: Centers for Medicare & Medicaid Services (CMS)**
Role: Provides federal guidance and oversight for Medicaid and Medicare-funded skilled services.
Agency: Pennsylvania Department of State
Role: Registers healthcare entities and ensures nurse licensure compliance.
2. SKILLED NURSING SERVICES OVERVIEW
Skilled Nursing Services are prescribed by a physician and delivered by a Registered Nurse (RN) or Licensed Practical Nurse (LPN) under physician oversight.
Approved providers may deliver:
Medication Administration: Injections, IV therapy, and oral medication management.
Wound Care: Dressing changes, pressure sore management, and surgical site care.
Chronic Condition Monitoring: Diabetes, cardiac, respiratory, or neurological support.
Post-Acute Care: Follow-up after hospital discharge or surgery.
Care Plan Development: RN-supervised care planning in coordination with the primary physician.
Training for Family/Caregivers: Teaching medication administration, monitoring signs/symptoms.
Documentation: Skilled nursing notes, medication logs, care plan updates, and billing forms.
3. LICENSING & PROVIDER APPROVAL REQUIREMENTS
Prerequisites:
Register your business with the Pennsylvania Department of State.
Obtain an EIN and Type 2 NPI.
Apply for a Home Health Agency License through the PA Department of Health (if operating a home health model).
Enroll with PROMISe™ as a Medicaid skilled nursing provider.
Contract with CHC MCOs for waiver-eligible populations.
Maintain malpractice, liability, and workers’ compensation insurance.
Develop a Skilled Nursing Services Policy & Procedure Manual in alignment with DOH and CMS guidelines.
4. PENNSYLVANIA PROVIDER ENROLLMENT PROCESS
Step 1: Form legal entity and obtain EIN, NPI, and required insurance.
Step 2: Apply for a Home Health Agency License via DOH (if applicable).
Step 3: Enroll with PROMISe™ under provider type for skilled nursing.
Step 4: Contract with CHC MCOs (UPMC, Keystone First, PA Health & Wellness).
Step 5: Submit staff credentials, licensure, and policy documentation.
Step 6: Begin receiving authorizations and referrals upon approval.
5. REQUIRED DOCUMENTATION
Business registration and Articles of Incorporation
EIN and NPI confirmation
Home Health License (if applicable)
Nursing staff licensure and credentials
Insurance certificates (malpractice, general liability, workers’ comp)
Skilled Nursing Policy & Procedure Manual including:
Plan of care development and clinical supervision
Medication administration and documentation protocols
Infection control and emergency response plans
HIPAA compliance and patient rights
RN and LPN supervisory requirements
Visit note templates and electronic documentation standards
Medicaid billing and chart audit readiness materials
6. STAFFING REQUIREMENTS
Role: Registered Nurse (RN)
Requirements: Active PA license; responsible for assessments, care planning, direct care, and LPN supervision.
Role: Licensed Practical Nurse (LPN)
Requirements: Active PA license; provides care under RN supervision.
Role: Clinical Supervisor / Director of Nursing
Requirements: Oversees nursing compliance, staff evaluations, and quality assurance.
All nursing staff must complete:
CPR/First Aid certification
HIPAA and abuse prevention training
Infection control and medication administration refreshers
Continuing education per PA Board of Nursing requirements
Electronic documentation and charting training
7. MEDICAID WAIVER PROGRAMS
Skilled Nursing Services are reimbursable through:
Medicaid State Plan Home Health Benefit – Physician-ordered nursing under medical necessity.
CHC Waiver (OLTL):
Skilled nursing included in service plan authorized by CHC MCOs
Aging, Independence, and OBRA Waivers (OLTL):
Nursing care to maintain or improve health at home
Children’s Waivers (if pediatric):
For medically complex children (via PH-95 or MA eligibility)
8. TIMELINE TO LAUNCH
Phase: Business Registration & Policy Manual Development
Timeline: 1–2 months
Phase: DOH Licensing & PROMISe™ Enrollment
Timeline: 2–4 months
Phase: MCO Contracting & Staff Credentialing
Timeline: 1–2 months
Phase: Referral Development & Service Launch
Timeline: Begins upon approval and readiness certification
9. CONTACT INFORMATION
PA Department of Health – Home Health Licensing
Website: https://www.health.pa.gov
PA DHS – Office of Long-Term Living (OLTL)
Website: https://www.dhs.pa.gov
PROMISe™ Provider Portal
Website: https://promise.dpw.state.pa.us
Community HealthChoices MCOs:
UPMC CHC – https://www.upmchealthplan.com
PA Health & Wellness – https://www.pahealthwellness.com
Keystone First CHC – https://www.keystonefirstchc.com
Centers for Medicare & Medicaid Services (CMS)
Website: https://www.cms.gov
WAIVER CONSULTING GROUP’S START-UP ASSISTANCE SERVICE — PENNSYLVANIA SKILLED NURSING PROVIDER
WCG supports healthcare agencies with launching, staffing, and maintaining high-quality skilled nursing operations in full compliance with PA Medicaid and licensing requirements.
Scope of Work:
Business registration, DOH licensing, and PROMISe™ enrollment
Policy & Procedure Manual development (aligned with clinical standards)
Nurse credentialing logs and supervision protocols
Visit note templates, medication tracking tools, and billing forms
MCO contracting guidance and referral development
Compliance tracking and audit readiness support

Adult Health
ADULT HEALTH SERVICES PROVIDER IN RHODE ISLAND
DELIVERING COMPREHENSIVE HEALTH, PERSONAL SUPPORT, AND WELLNESS SERVICES TO ADULTS WITH DISABILITIES, CHRONIC CONDITIONS, OR AGE-RELATED NEEDS
Adult Health Services in Rhode Island encompass a broad array of Medicaid-funded supports for adults who require ongoing assistance with personal care, medical monitoring, and wellness activities. These services are primarily delivered in home-based or community settings and are authorized through the Rhode Island Medicaid State Plan, 1115 Global Waiver, and various Home and Community-Based Services (HCBS) Waivers. Adult health supports are designed to prevent institutionalization, promote independence, and maintain overall health and well-being.
1. GOVERNING AGENCIES
Agency: Rhode Island Executive Office of Health and Human Services (EOHHS)
Role: Administers Medicaid programs and waiver services, processes provider enrollment and service authorizations.
Agency: Rhode Island Department of Health (RIDOH)**
Role: Licenses healthcare and home care agencies, regulates nursing and personal care standards.
Agency: Department of Behavioral Healthcare, Developmental Disabilities & Hospitals (BHDDH)**
Role: Authorizes adult health services for individuals with intellectual/developmental disabilities under HCBS waivers.
Agency: Centers for Medicare & Medicaid Services (CMS)**
Role: Sets federal guidelines for Medicaid services, including home-based care and adult wellness supports.
2. ADULT HEALTH SERVICES OVERVIEW
Adult Health Services are non-institutional supports aimed at helping adults maintain or improve their functional status, manage chronic conditions, and live independently.
Approved providers may deliver:
Skilled Nursing Care: Medication administration, wound care, chronic condition management.
Personal Care Services: Assistance with bathing, grooming, dressing, mobility, and toileting.
Health Monitoring: Vital signs, symptom tracking, and medication adherence.
Nutritional Support: Meal planning, preparation, feeding assistance, and dietary monitoring.
Home Health Aide Services: Supervised in-home assistance with ADLs and IADLs.
Adult Day Health (optional): Structured care during the day with meals, nursing oversight, and activities.
Respite & Companion Services: Temporary relief for caregivers and social support for isolated adults.
Therapy Coordination: Referrals for PT/OT/ST and behavioral support as needed.
Documentation: Care plans, shift notes, incident reports, and Medicaid billing logs.
3. LICENSING & PROVIDER APPROVAL REQUIREMENTS
Prerequisites:
Register your business with the Rhode Island Secretary of State.
Obtain an EIN and Type 2 NPI.
Apply for licensure through RIDOH if delivering skilled or in-home care services.
Enroll as a Medicaid provider through EOHHS or the RI provider portal.
Submit an Adult Health Services Policy & Procedure Manual for approval (if required).
Maintain insurance (liability, workers’ comp, malpractice for skilled care).
4. RHODE ISLAND PROVIDER ENROLLMENT PROCESS
Step 1: Register your business and secure RIDOH licensure (if applicable).
Step 2: Apply to become a Medicaid provider under appropriate service codes.
Step 3: Submit service descriptions, staff qualifications, and care protocols.
Step 4: Pass readiness checks or site inspections (for in-home and adult day health providers).
Step 5: Begin service delivery upon authorization.
5. REQUIRED DOCUMENTATION
Articles of Incorporation and EIN/NPI confirmations
RIDOH licensure certificate (for applicable services)
Insurance certificates (general, workers’ comp, malpractice)
Adult Health Services Policy & Procedure Manual including:
Care planning and service delivery protocols
Documentation and billing standards
Medication safety and emergency procedures
Staff supervision and training guidelines
Participant rights, HIPAA compliance, and incident reporting
Quality assurance and participant feedback tools
6. STAFFING REQUIREMENTS
Role: Registered Nurse (RN)
Requirements: RI licensure, CPR certification, care coordination experience.
Role: Certified Nursing Assistant (CNA) / Home Health Aide (HHA)
Requirements: RIDOH certification, CPR/First Aid, background check.
Role: Adult Day Program Coordinator (if applicable)
Requirements: Program oversight, staff management, and compliance knowledge.
Optional: Licensed Therapists (PT/OT/ST)
Requirements: Licensed in RI; required only if therapy is provided directly.
All staff must complete:
HIPAA and confidentiality training
Abuse prevention and mandatory reporting
Participant engagement and dignity-in-care training
Emergency preparedness and infection control
Annual performance reviews and skills assessments
7. MEDICAID WAIVER PROGRAMS
Adult Health Services are offered through:
Medicaid State Plan (PCA, HHA, RN/LPN Services)
1115 Global Waiver (HCBS): Covers adult health services in home and day settings
BHDDH IDD Waivers: Authorizes care for adults with disabilities living in the community
Katie Beckett/TEFRA (for transition-aged youth)
Self-Directed Waiver Supports: Participants can choose their own providers of adult health services
8. TIMELINE TO LAUNCH
Phase: Business Formation & Policy Manual Development
Timeline: 1–2 months
Phase: RIDOH Licensing & Medicaid Enrollment
Timeline: 2–3 months
Phase: Staff Hiring & Service Setup
Timeline: 30–60 days
Phase: Readiness Review & Participant Referrals
Timeline: Begins once enrollment and authorization are approved
9. CONTACT INFORMATION
Rhode Island Executive Office of Health and Human Services (EOHHS)
Website: https://eohhs.ri.gov
Rhode Island Department of Health (RIDOH)
Website: https://health.ri.gov
Rhode Island Medicaid Provider Portal
Website: https://www.riproviderportal.org
Department of Behavioral Healthcare, Developmental Disabilities & Hospitals (BHDDH)
Website: https://bhddh.ri.gov
Centers for Medicare & Medicaid Services (CMS)
Website: https://www.cms.gov
WAIVER CONSULTING GROUP’S START-UP ASSISTANCE SERVICE — RHODE ISLAND ADULT HEALTH SERVICES PROVIDER
WCG supports adult health service providers in Rhode Island with compliance, documentation, and Medicaid startup to deliver high-quality care in homes and communities.
Scope of Work:
RIDOH licensure and Medicaid enrollment guidance
Customized Adult Health Policy & Procedure Manual
RN/CNA credentialing tools and shift documentation logs
Service delivery templates and care plan samples
Participant rights and incident tracking tools
Billing training and Medicaid documentation workflows
Assistive Technology
ASSISTIVE TECHNOLOGY SERVICES PROVIDER IN RHODE ISLAND
ENHANCING INDEPENDENCE AND ACCESSIBILITY FOR INDIVIDUALS WITH DISABILITIES THROUGH INNOVATIVE SUPPORTIVE DEVICES AND TECHNOLOGIES
Assistive Technology (AT) Services in Rhode Island are Medicaid-funded supports designed to increase, maintain, or improve the functional capabilities of individuals with disabilities or chronic conditions. These services may include the evaluation, purchase, customization, and training for devices that support mobility, communication, daily living, or safety. AT services are available through Rhode Island’s Medicaid 1115 Waiver, Developmental Disability (DD) Waivers, and Long-Term Services and Supports (LTSS) programs.
1. GOVERNING AGENCIES
Agency: Rhode Island Executive Office of Health and Human Services (EOHHS)
Role: Oversees Medicaid policy, funding, and service authorizations for assistive technology.
Agency: Department of Behavioral Healthcare, Developmental Disabilities & Hospitals (BHDDH)
Role: Manages AT approvals under DD Waivers, including equipment assessments and funding coordination.
Agency: Centers for Medicare & Medicaid Services (CMS)**
Role: Provides federal guidelines and oversight of Medicaid-funded AT under 1915(c) and 1115 waivers.
Agency: Rhode Island Department of Health (RIDOH)**
Role: May regulate medical equipment distributors or clinical providers involved in AT assessments or customization.
2. ASSISTIVE TECHNOLOGY SERVICES OVERVIEW
Assistive technology includes any item or system used to improve the independence, communication, safety, or participation of individuals with functional impairments.
Approved providers may deliver:
AT Needs Assessment: Evaluation by a qualified clinician to determine appropriate technologies.
Device Selection & Procurement: Sourcing Medicaid-approved AT items, including mobility aids, adaptive switches, and communication devices.
Device Installation & Customization: Fitting or modifying AT devices to meet individual needs.
Training & Support: Teaching the individual, caregivers, or staff to use the AT safely and effectively.
Maintenance & Repair: Ensuring devices remain functional and safe for use.
Documentation: Evaluation reports, service delivery logs, and Medicaid billing templates.
3. LICENSING & PROVIDER APPROVAL REQUIREMENTS
Prerequisites:
Register your business with the Rhode Island Secretary of State.
Obtain a Federal EIN and Type 2 NPI.
Enroll in the Rhode Island Medicaid system as an AT provider.
If providing clinical services (e.g., OT/PT/speech evaluation), staff must hold valid RI licensure.
Maintain liability insurance and, if applicable, durable medical equipment (DME) vendor compliance.
Develop an Assistive Technology Services Policy & Procedure Manual covering assessment, delivery, training, and compliance standards.
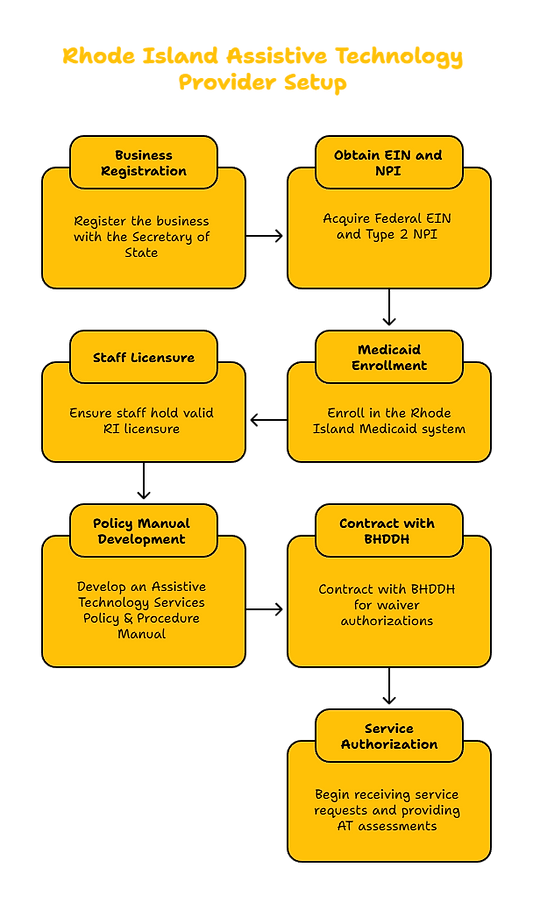
4. RHODE ISLAND PROVIDER ENROLLMENT PROCESS
Step 1: Register your business entity, EIN, and obtain NPI.
Step 2: Apply for Medicaid provider enrollment through the RI EOHHS provider portal.
Step 3: Submit staff licensure (if applicable), service descriptions, and your policy manual.
Step 4: Contract with BHDDH or Medicaid MCOs for waiver authorizations.
Step 5: Begin receiving service requests and providing AT assessments and device installations.
5. REQUIRED DOCUMENTATION
Articles of Incorporation and business registration
EIN and NPI confirmation
Insurance certificates (liability, workers’ comp, and DME vendor policies if applicable)
Staff licenses (OTs, PTs, Speech Therapists, Assistive Tech Specialists)
AT Services Policy & Procedure Manual including:
Assessment tools and authorization workflows
AT procurement and delivery protocols
Participant training guides and follow-up visit notes
Device customization and maintenance logs
Medicaid billing formats and tracking
HIPAA and participant safety compliance policies
6. STAFFING REQUIREMENTS
Role: Assistive Technology Specialist / Technician
Requirements: Training in AT devices and modifications; experience with disability-related technology.
Role: Licensed Therapist (OT, PT, SLP)
Requirements: State license required for device evaluations and therapeutic justification.
Role: Program Coordinator / Case Manager
Requirements: Oversees referrals, schedules evaluations, and manages equipment logistics.
All staff must complete:
HIPAA training and confidentiality assurance
Safety procedures and infection control for shared devices
Documentation and Medicaid billing protocol training
Cultural competence and client-centered communication
7. MEDICAID WAIVER PROGRAMS
AT Services are funded through:
Global Consumer Choice Compact (1115 Waiver): Covers medically necessary assistive devices and training under HCBS.
BHDDH DD Waivers: Authorize AT assessments, customization, and training for individuals with developmental disabilities.
LTSS Medicaid Managed Care: AT available as a support for adults receiving home and community-based services.
Early Intervention / Pediatric Waivers: Limited AT funding available through specialized child health programs.
8. TIMELINE TO LAUNCH
Phase: Business Formation & Manual Development
Timeline: 1–2 months
Phase: Medicaid Enrollment & MCO/BHDDH Contracting
Timeline: 2–3 months
Phase: Staff Credentialing & Training
Timeline: 30–60 days
Phase: Service Authorization & Launch
Timeline: Begins once approvals and AT referrals are received
9. CONTACT INFORMATION
Rhode Island Executive Office of Health and Human Services (EOHHS)
Website: https://eohhs.ri.gov
Rhode Island Medicaid Provider Portal
Website: https://www.riproviderportal.org
Department of Behavioral Healthcare, Developmental Disabilities & Hospitals (BHDDH)
Website: https://bhddh.ri.gov
Centers for Medicare & Medicaid Services (CMS)
Website: https://www.cms.gov
RI Department of Health – Licensure and DME Vendors
Website: https://health.ri.gov
WAIVER CONSULTING GROUP’S START-UP ASSISTANCE SERVICE — RHODE ISLAND ASSISTIVE TECHNOLOGY PROVIDER
WCG helps AT providers navigate licensure, Medicaid enrollment, and service setup to meet Rhode Island’s growing demand for individualized technology solutions.
Scope of Work:
Business registration and Medicaid enrollment support
Policy & Procedure Manual tailored to AT evaluations and delivery
Staff credentialing tools and training logs
AT evaluation templates and documentation workflows
Authorization tracking and Medicaid billing resources
Contracting support with BHDDH and Medicaid managed care plans
Behavioral Health
BEHAVIORAL HEALTH SERVICES PROVIDER IN RHODE ISLAND
PROMOTING EMOTIONAL WELL-BEING, MENTAL HEALTH STABILITY, AND RECOVERY THROUGH COMMUNITY-BASED BEHAVIORAL SUPPORTS
Behavioral Health Services in Rhode Island address the emotional, psychological, and psychiatric needs of individuals across the lifespan. These services are funded through Rhode Island Medicaid (including the 1115 Global Waiver), State Plan, and various federal initiatives. Providers support individuals with mental illness, substance use disorders, or behavioral challenges through therapeutic interventions, counseling, crisis stabilization, and recovery supports in home and community settings.
1. GOVERNING AGENCIES
Agency: Rhode Island Executive Office of Health and Human Services (EOHHS)
Role: Oversees Medicaid funding, behavioral health benefits, and provider enrollment.
Agency: Department of Behavioral Healthcare, Developmental Disabilities & Hospitals (BHDDH)
Role: Licenses mental health and substance use disorder providers and monitors behavioral service delivery.
Agency: Rhode Island Department of Health (RIDOH)**
Role: Regulates licensed mental health professionals and behavioral health facilities.
Agency: Centers for Medicare & Medicaid Services (CMS)**
Role: Sets national standards for behavioral health under Medicaid and HCBS programs.
2. BEHAVIORAL HEALTH SERVICES OVERVIEW
These services support people with mental health diagnoses, emotional disorders, or behavioral concerns impacting daily life. Services are person-centered, trauma-informed, and aligned with evidence-based practices.
Approved providers may deliver:
Individual & Group Therapy: CBT, DBT, trauma-focused therapy, and grief counseling.
Psychiatric Evaluation & Medication Management: Diagnosis, prescribing, and symptom monitoring by licensed clinicians.
Mobile Crisis Response & Crisis Stabilization: Immediate intervention in homes or community settings.
Behavioral Support Services (BSS): In-home behavior planning and coaching for individuals with IDD or dual diagnoses.
Peer Recovery Support: Peer mentoring for those in mental health or substance use recovery.
Case Management: Coordination of housing, transportation, medical care, and benefits.
Integrated Primary & Behavioral Health Care: Coordination between mental health and physical health providers.
Documentation & Billing: Behavioral health assessments, treatment plans, and encounter notes.
3. LICENSING & PROVIDER APPROVAL REQUIREMENTS
Prerequisites:
Register your business with the RI Secretary of State.
Obtain EIN and Type 2 NPI.
Secure BHDDH licensure for mental health or substance use treatment services (as applicable).
Enroll in Medicaid through the EOHHS provider portal.
Employ credentialed clinicians (LICSW, LMHC, PsyD, MD, etc.) and paraprofessionals (e.g., BSS).
Develop a Behavioral Health Services Policy & Procedure Manual covering service models, clinical protocols, safety, and documentation.
4. RHODE ISLAND PROVIDER ENROLLMENT PROCESS
Step 1: Form your legal business, obtain EIN, and NPI.
Step 2: Apply for BHDDH behavioral health licensure based on services (outpatient, residential, etc.).
Step 3: Submit Medicaid enrollment application with required credentials and manuals.
Step 4: Ensure staff meet professional and Medicaid requirements.
Step 5: Begin receiving referrals and service authorizations.
5. REQUIRED DOCUMENTATION
Business registration and licensure certificates
Medicaid and BHDDH enrollment confirmation
Staff licenses, background checks, and supervision logs
Insurance (liability, malpractice, workers’ comp)
Behavioral Health Policy & Procedure Manual including:
Risk assessments, treatment plan formats, and diagnostic criteria
Emergency response and suicide prevention protocols
HIPAA compliance and participant rights documentation
Crisis intervention procedures and de-escalation training
Quality assurance, peer review, and staff supervision protocols
Medicaid-compliant progress notes and billing documentation
6. STAFFING REQUIREMENTS
Role: Licensed Mental Health Clinician (LICSW, LMHC, LPC)
Requirements: Active RI license, clinical supervision plan (if required), Medicaid enrollment.
Role: Psychiatrist / Prescribing Provider
Requirements: RI licensure (MD or APRN), DEA registration, and psychiatric specialization.
Role: Behavioral Support Specialist (BSS)
Requirements: Experience in behavior plans, often supervised by licensed clinician.
Role: Peer Recovery Specialist
Requirements: State-approved peer training, lived experience, background check.
Role: Case Manager / Care Coordinator
Requirements: Bachelor’s degree or experience in human services, trained in system navigation.
All staff must complete:
HIPAA and documentation training
Trauma-informed care and cultural competence
Safety, abuse prevention, and crisis response
Treatment planning and evidence-based practice implementation
Mandatory reporting and emergency procedures
7. MEDICAID WAIVER PROGRAMS
Behavioral Health Services may be funded through:
Medicaid State Plan Services – Outpatient therapy, psychiatry, case management
1115 Global Waiver (HCBS) – Behavioral supports for adults and youth in community settings
BHDDH DD Waivers – Behavioral support for individuals with IDD
Katie Beckett/TEFRA – In-home therapy for children with complex needs
Crisis Intervention and Wraparound Programs – State-funded or braided with Medicaid
8. TIMELINE TO LAUNCH
Phase: Business Formation & Manual Development
Timeline: 1–2 months
Phase: BHDDH Licensing & Medicaid Enrollment
Timeline: 2–3 months
Phase: Staff Hiring, Credentialing & Clinical Setup
Timeline: 30–60 days
Phase: Service Authorization & Participant Intake
Timeline: Begins once staff are active and referrals are assigned
9. CONTACT INFORMATION
Rhode Island Executive Office of Health and Human Services (EOHHS)
Website: https://eohhs.ri.gov
Rhode Island Department of Health (RIDOH)
Website: https://health.ri.gov
Department of Behavioral Healthcare, Developmental Disabilities & Hospitals (BHDDH)
Licensing Portal: https://bhddh.ri.gov
Rhode Island Medicaid Provider Portal
Website: https://www.riproviderportal.org
Centers for Medicare & Medicaid Services (CMS)
Website: https://www.cms.gov
WAIVER CONSULTING GROUP’S START-UP ASSISTANCE SERVICE — RHODE ISLAND BEHAVIORAL HEALTH PROVIDER
WCG guides behavioral health providers through the compliance, clinical, and Medicaid setup process to launch trauma-informed, recovery-oriented services.
Scope of Work:
BHDDH licensing and Medicaid enrollment support
Behavioral Health Policy & Procedure Manual creation
Clinical documentation templates and treatment plan formats
Credentialing workflows and staff compliance trackers
Crisis protocols, risk management tools, and audit prep
Medicaid billing setup and progress note structure

Home Modification
HOME MODIFICATION SERVICES PROVIDER IN RHODE ISLAND
MAKING HOMES SAFER AND MORE ACCESSIBLE FOR INDIVIDUALS WITH DISABILITIES, AGING NEEDS, AND MOBILITY LIMITATIONS
Home Modification Services in Rhode Island provide physical adaptations to a person’s primary residence to ensure accessibility, safety, and independence. These services are authorized through Medicaid Home and Community-Based Services (HCBS) under the 1115 Global Waiver, BHDDH IDD Waivers, and certain pediatric and aging-related supports. Modifications are typically non-routine and must be related to the individual’s disability or functional limitations.
1. GOVERNING AGENCIES
Agency: Rhode Island Executive Office of Health and Human Services (EOHHS)
Role: Manages Medicaid funding and authorizes home modifications under HCBS waiver programs.
Agency: Department of Behavioral Healthcare, Developmental Disabilities & Hospitals (BHDDH)
Role: Coordinates waiver-based home modifications for individuals with developmental disabilities.
Agency: Rhode Island Department of Health (RIDOH)**
Role: May oversee compliance for contractors providing work involving structural or health-related features.
Agency: Centers for Medicare & Medicaid Services (CMS)**
Role: Regulates HCBS waiver spending and defines allowable home modifications under federal guidelines.
2. HOME MODIFICATION SERVICES OVERVIEW
These services adapt a participant’s living environment to support their health, functional needs, and ability to remain in the community.
Approved providers may deliver:
Mobility Enhancements: Ramps, widened doorways, stair glides, platform lifts.
Bathroom Modifications: Roll-in showers, grab bars, accessible toilets, sink adjustments.
Environmental Controls: Voice-activated lighting, door openers, and smart-home safety devices.
Kitchen Accessibility: Lowered counters, accessible appliances, turn-knob adaptations.
Entry and Exit Safety Features: Non-slip flooring, handrails, levered door handles.
Structural Changes: Based on ISP and authorized by a clinician or waiver case manager.
Maintenance (Limited): Repairs to existing authorized modifications.
Documentation: Pre-approval request packets, scope of work, and proof of completion.
3. LICENSING & PROVIDER APPROVAL REQUIREMENTS
Prerequisites:
Register your business with the RI Secretary of State.
Obtain EIN and Type 2 NPI (if billing Medicaid directly).
Enroll with EOHHS as a Home Modification or Environmental Adaptation provider.
For waiver-funded clients (IDD or aging), coordinate with BHDDH or waiver case managers.
Contract with licensed contractors, plumbers, and electricians (as needed).
Develop a Home Modification Services Policy & Procedure Manual covering installation standards, safety, and compliance.
4. RHODE ISLAND PROVIDER ENROLLMENT PROCESS
Step 1: Establish your business entity, secure EIN/NPI, and insurance.
Step 2: Apply to become a Medicaid provider under home modification or assistive service categories.
Step 3: Submit proof of contractor licensing (if applicable) and sample project scopes.
Step 4: Partner with case managers to receive service requests and site assessments.
Step 5: Complete installations upon authorization and submit documentation for reimbursement.
5. REQUIRED DOCUMENTATION
Business registration and EIN/NPI confirmations
Proof of contractor licenses and subcontractor agreements
Medicaid enrollment confirmation
Insurance certificates (general liability, workers’ comp, product liability)
Home Modification Policy & Procedure Manual including:
Authorization procedures and scope of work templates
Safety and compliance checklists
Participant consent and satisfaction forms
Warranty policies and follow-up protocols
Progress reporting and invoicing templates
HIPAA, privacy, and incident tracking procedures
6. STAFFING REQUIREMENTS
Role: Home Modification Specialist / Coordinator
Requirements: Project planning, site assessments, Medicaid documentation experience.
Role: Licensed Contractor / Installer
Requirements: Valid RI contractor license, ADA compliance training preferred.
Role: Occupational Therapist (as consultant, optional)
Requirements: Licensed OT to assess adaptive needs and recommend modifications.
All staff or subcontractors must adhere to:
OSHA safety regulations
HCBS and ADA accessibility guidelines
Background checks for workers entering participants’ homes
HIPAA confidentiality and abuse prevention training
7. MEDICAID WAIVER PROGRAMS
Home Modification Services are authorized under:
1115 Global Waiver (HCBS) – For adults needing physical home adaptations to remain independent
BHDDH DD Waivers – For individuals with developmental disabilities needing accessibility supports
Katie Beckett/TEFRA Program – Pediatric modifications (e.g., roll-in showers, lifts)
Self-Directed Waivers – Participants may select their own home modification providers from an approved list
State Plan (Limited) – For specific medical necessity-based items coordinated with DME
8. TIMELINE TO LAUNCH
Phase: Business Registration & Policy Manual Development
Timeline: 1–2 months
Phase: Medicaid Enrollment & Licensing (Contractor Partnerships)
Timeline: 1–2 months
Phase: Team Setup & Referral Network Development
Timeline: 30–60 days
Phase: Begin Assessments & Installations
Timeline: Upon receiving service authorization and approval
9. CONTACT INFORMATION
Rhode Island Executive Office of Health and Human Services (EOHHS)
Website: https://eohhs.ri.gov
Department of Behavioral Healthcare, Developmental Disabilities & Hospitals (BHDDH)
Website: https://bhddh.ri.gov
Rhode Island Medicaid Provider Portal
Website: https://www.riproviderportal.org
Rhode Island Department of Health (RIDOH)
Website: https://health.ri.gov
Centers for Medicare & Medicaid Services (CMS)
Website: https://www.cms.gov
WAIVER CONSULTING GROUP’S START-UP ASSISTANCE SERVICE — RHODE ISLAND HOME MODIFICATION PROVIDER
WCG helps providers launch compliant home modification services that improve accessibility and quality of life for Rhode Island Medicaid recipients.
Scope of Work:
Medicaid enrollment and waiver-based service authorization guidance
Partnership development with licensed contractors
Home Modification Policy & Procedure Manual
Safety inspection checklists and consent forms
Pre- and post-installation documentation tools
Billing templates, HIPAA compliance, and incident response workflows

Nursing Facility Transition
NURSING FACILITY TRANSITION SERVICES PROVIDER IN RHODE ISLAND
SUPPORTING INDIVIDUALS TO SAFELY TRANSITION FROM INSTITUTIONAL CARE TO INDEPENDENT, COMMUNITY-BASED LIVING WITH DIGNITY AND CHOICE
Nursing Facility Transition (NFT) Services in Rhode Island assist individuals in moving from nursing homes or institutional settings back into the community. These Medicaid-funded services are designed to support older adults and individuals with disabilities who are eligible for Home and Community-Based Services (HCBS) but require planning, coordination, and supports to successfully live in a home or residential setting. NFT services are available under Rhode Island’s Medicaid 1115 Waiver and managed through the Executive Office of Health and Human Services (EOHHS), Long-Term Services and Supports (LTSS), and Medicaid Managed Care Organizations.
1. GOVERNING AGENCIES
Agency: Rhode Island Executive Office of Health and Human Services (EOHHS)
Role: Administers Medicaid-funded transition programs, oversees provider enrollment and payments.
Agency: Nursing Facility Transition Coordinators / Medicaid MCOs
Role: Coordinate discharge planning and refer individuals for transition services.
Agency: Centers for Medicare & Medicaid Services (CMS)**
Role: Regulates Medicaid HCBS transition services and 1115 demonstration programs.
Agency: Rhode Island Department of Health (RIDOH)**
Role: Licenses providers if offering home health, personal care, or housing support components as part of transition.
2. NURSING FACILITY TRANSITION SERVICES OVERVIEW
NFT Services support individuals preparing to leave a nursing facility and reintegrate into the community by addressing housing, personal supports, environmental accessibility, and care coordination.
Approved providers may deliver:
Individualized Transition Planning: Housing search, benefit applications, and discharge coordination.
Community Support Setup: Linking individuals with in-home care providers, adult day services, or Medicaid waivers.
Housing Stabilization Services: Security deposit, utility setup, or short-term tenancy support (when authorized).
Home Modifications & Equipment Coordination: Ensuring safety and accessibility post-discharge.
Life Skills Coaching: Budgeting, grocery shopping, medication self-management.
Follow-Up Support: Regular visits to ensure stability and service continuity post-transition.
Documentation: Transition plan, service log, and billing records.
3. LICENSING & PROVIDER APPROVAL REQUIREMENTS
Prerequisites:
Register your business entity with the Rhode Island Secretary of State.
Obtain a Federal EIN and Type 2 NPI.
Enroll as a Medicaid provider for Home and Community-Based Services (HCBS) under NFT codes.
If providing direct care (e.g., homemaker, personal care, clinical), obtain RIDOH licensure.
Maintain liability, workers’ comp, and general business insurance.
Develop a Nursing Facility Transition Policy & Procedure Manual compliant with EOHHS and CMS guidelines.
4. RHODE ISLAND PROVIDER ENROLLMENT PROCESS
Step 1: Register your business, obtain EIN and NPI, and secure insurance.
Step 2: Enroll in the Medicaid provider portal and apply for NFT-related service codes.
Step 3: Contract with Medicaid MCOs or referral networks handling transition coordination.
Step 4: Submit documentation including your manual, staff resumes, and service structure.
Step 5: Upon approval, begin receiving referrals for transition candidates.
5. REQUIRED DOCUMENTATION
Articles of Incorporation and business registration
EIN and NPI confirmations
Medicaid enrollment confirmation
RIDOH licensure (if applicable to care components)
Nursing Facility Transition Policy & Procedure Manual including:
Transition planning workflows and checklists
Housing coordination and referral documentation
Post-discharge follow-up and service monitoring
Risk mitigation and safety planning procedures
Client rights, privacy policies, and HIPAA compliance
Medicaid billing templates and transition reporting forms
6. STAFFING REQUIREMENTS
Role: Transition Coordinator / Case Manager
Requirements: Experience with discharge planning, community resources, and Medicaid benefits.
Role: Housing Specialist (optional)
Requirements: Knowledge of rental navigation, vouchers, and tenant-landlord negotiation.
Role: Direct Support Worker or HHA (if providing in-home support)
Requirements: Background check, CPR/First Aid, and training in ADL assistance.
All staff must complete:
HIPAA and participant rights training
Risk mitigation and emergency planning training
Housing and benefits coordination education
Documentation and Medicaid billing training
Cultural competency and trauma-informed care (recommended)
7. MEDICAID WAIVER PROGRAMS
NFT Services are authorized through:
Global Consumer Choice Compact 1115 Waiver (RI Medicaid): Includes NFT supports under HCBS.
LTSS Managed Care (MCOs): Transition services integrated into case management contracts.
Developmental Disability Waivers (via BHDDH): Include transitions for eligible individuals with ID/DD.
Money Follows the Person (MFP) Demonstration (if reactivated): Formerly provided enhanced transition supports.
8. TIMELINE TO LAUNCH
Phase: Business Formation & Manual Development
Timeline: 1–2 months
Phase: Medicaid Enrollment & RIDOH Licensing (if needed)
Timeline: 2–3 months
Phase: Staff Hiring, Training & Readiness Prep
Timeline: 30–60 days
Phase: Referral Activation & Service Start
Timeline: Begins after enrollment and referral network setup
9. CONTACT INFORMATION
Rhode Island Executive Office of Health and Human Services (EOHHS)
Website: https://eohhs.ri.gov
Rhode Island Medicaid Provider Portal
Website: https://www.riproviderportal.org
Rhode Island Department of Health (RIDOH) – Licensure Info
Website: https://health.ri.gov/licenses
Centers for Medicare & Medicaid Services (CMS)
Website: https://www.cms.gov
WAIVER CONSULTING GROUP’S START-UP ASSISTANCE SERVICE — RHODE ISLAND NFT SERVICES PROVIDER
WCG supports new and existing providers in Rhode Island launching Medicaid-authorized transition services that bridge institutional and community-based care.
Scope of Work:
Business registration and Medicaid enrollment
NFT-specific Policy & Procedure Manual development
Staff training plans and transition documentation templates
Housing resource guides and referral workflows
Contracting support with Medicaid MCOs and DD networks
Billing tools, readiness checklists, and incident protocols

Community Integration
COMMUNITY INTEGRATION SERVICES PROVIDER IN RHODE ISLAND
SUPPORTING MEANINGFUL PARTICIPATION IN DAILY LIFE, SOCIAL ACTIVITIES, AND COMMUNITY SETTINGS FOR INDIVIDUALS WITH DISABILITIES OR LONG-TERM SUPPORT NEEDS
Community Integration Services in Rhode Island empower individuals with intellectual/developmental disabilities (IDD), behavioral health needs, or chronic conditions to participate fully in everyday community life. These Medicaid-funded supports are authorized under the 1115 Global Waiver, BHDDH IDD Waivers, and other Home and Community-Based Services (HCBS) programs. The goal is to reduce isolation and promote independence through community engagement and skill-building.
1. GOVERNING AGENCIES
Agency: Rhode Island Executive Office of Health and Human Services (EOHHS)
Role: Administers Medicaid and authorizes HCBS funding for integration services.
Agency: Department of Behavioral Healthcare, Developmental Disabilities & Hospitals (BHDDH)
Role: Authorizes Community-Based Supports and oversees provider standards under DD Waivers.
Agency: Rhode Island Department of Health (RIDOH)**
Role: May regulate health-related aspects of service environments (as needed).
Agency: Centers for Medicare & Medicaid Services (CMS)**
Role: Ensures HCBS programs comply with federal settings rules and person-centered planning.
2. COMMUNITY INTEGRATION SERVICES OVERVIEW
These services focus on supporting individuals in building social skills, accessing public spaces, volunteering, working, and participating in inclusive settings outside their homes.
Approved providers may deliver:
Community Mapping & Planning: Identifying individual goals for integration (e.g., employment, recreation, worship).
Skill-Building Activities: Travel training, communication support, financial literacy, and safety in the community.
Peer Interaction & Social Coaching: Facilitating friendships, group outings, and positive behavior reinforcement.
Access Support: Navigating transportation, community resources, and public programs.
Civic Participation: Assistance with voting, advocacy events, and volunteering.
Documentation: Individual Service Plans (ISPs), activity logs, and community participation reports.
3. LICENSING & PROVIDER APPROVAL REQUIREMENTS
Prerequisites:
Register your organization with the Rhode Island Secretary of State.
Obtain EIN and Type 2 NPI.
Apply to BHDDH for approval as a provider of Community-Based Supports (for IDD population).
Enroll in Medicaid through the EOHHS provider portal.
Submit service delivery model, staffing plan, and integration activity procedures.
Develop a Community Integration Services Policy & Procedure Manual aligned with HCBS Settings Rule and participant choice.
4. RHODE ISLAND PROVIDER ENROLLMENT PROCESS
Step 1: Register your business, obtain EIN, NPI, and insurance.
Step 2: Apply to BHDDH as a provider of community-based waiver services.
Step 3: Submit staffing qualifications and community participation procedures.
Step 4: Enroll with Medicaid and receive service authorization through ISPs.
Step 5: Begin service delivery with ongoing documentation and review.
5. REQUIRED DOCUMENTATION
Business registration, EIN/NPI confirmations
BHDDH provider approval letter
Insurance certificates (liability, workers’ comp)
Medicaid enrollment documentation
Community Integration Policy & Procedure Manual including:
ISP-driven goal development and support plans
Community access and safety protocols
Supervision and group activity procedures
Progress tracking, outcome measurement, and satisfaction surveys
Transportation coordination and public safety planning
HIPAA, participant rights, and incident reporting standards
6. STAFFING REQUIREMENTS
Role: Community Integration Specialist / Support Worker
Requirements: Experience with disability supports, background check, CPR/First Aid, training in person-centered planning.
Role: Program Supervisor / Coordinator
Requirements: Oversight of staff, ISP implementation, and documentation reviews.
Role (optional): Behavioral Consultant
Requirements: For clients with behavior plans, typically licensed or experienced in behavior support.
All staff must complete:
HCBS Settings Rule and dignity in care training
Abuse prevention and incident response
Community navigation and risk reduction strategies
Documentation and Medicaid billing compliance
Cultural competence and trauma-informed care education
7. MEDICAID WAIVER PROGRAMS
Community Integration Services are covered under:
BHDDH DD Waivers (Community-Based Supports): For individuals with intellectual and developmental disabilities
1115 Global Waiver (HCBS): Authorizes non-clinical supports for adult community living
Katie Beckett/TEFRA (Limited): For children in specific home and community support arrangements
Self-Directed Supports Waivers: Participants choose community providers for integration services
8. TIMELINE TO LAUNCH
Phase: Business Formation & Policy Manual Creation
Timeline: 1–2 months
Phase: BHDDH and Medicaid Enrollment
Timeline: 2–3 months
Phase: Staff Hiring & Training
Timeline: 30–60 days
Phase: Participant ISP Alignment & Service Initiation
Timeline: Begins after service authorizations are received
9. CONTACT INFORMATION
Rhode Island Executive Office of Health and Human Services (EOHHS)
Website: https://eohhs.ri.gov
Department of Behavioral Healthcare, Developmental Disabilities & Hospitals (BHDDH)
Website: https://bhddh.ri.gov
Rhode Island Medicaid Provider Portal
Website: https://www.riproviderportal.org
Rhode Island Department of Health (RIDOH)
Website: https://health.ri.gov
Centers for Medicare & Medicaid Services (CMS)
Website: https://www.cms.gov
WAIVER CONSULTING GROUP’S START-UP ASSISTANCE SERVICE — RHODE ISLAND COMMUNITY INTEGRATION PROVIDER
WCG supports providers launching integration services focused on empowering individuals to thrive in inclusive community environments.
Scope of Work:
BHDDH and Medicaid enrollment guidance
Community Integration Policy & Procedure Manual
ISP-aligned service delivery tools and activity logs
Staff training templates and safety protocols
Participant choice documentation and progress trackers
Compliance audits and HCBS Settings Rule alignment

TEFRA Program
TEFRA PROGRAM (TAX EQUITY AND FISCAL RESPONSIBILITY ACT) — RHODE ISLAND
ENABLING CHILDREN WITH DISABILITIES TO RECEIVE MEDICAID SUPPORT WHILE LIVING AT HOME — REGARDLESS OF PARENTAL INCOME
The TEFRA-like Program in Rhode Island (also known as Katie Beckett eligibility) allows children with significant disabilities or complex medical needs to qualify for Medicaid based solely on the child’s income and assets—not the parents’. This program enables families to access necessary medical and support services at home, rather than requiring institutional placement for Medicaid eligibility. Administered through the Executive Office of Health and Human Services (EOHHS), TEFRA aligns with federal provisions outlined in Section 134 of the Tax Equity and Fiscal Responsibility Act of 1982.
1. GOVERNING AGENCIES
Agency: Rhode Island Executive Office of Health and Human Services (EOHHS)
Role: Determines eligibility, manages applications, and authorizes Medicaid services under the Katie Beckett provision.
Agency: Centers for Medicare & Medicaid Services (CMS)**
Role: Oversees federal Medicaid policies including TEFRA-related eligibility standards.
Agency: Rhode Island Department of Human Services (DHS)**
Role: May assist in outreach, enrollment support, and coordination of wraparound services.
2. TEFRA PROGRAM OVERVIEW
The TEFRA/Katie Beckett option is designed for children under age 19 who:
Have a qualifying disability or complex medical condition (as determined by SSI standards)
Require institutional-level care but can be safely supported at home
Would not otherwise qualify for Medicaid due to family income
Live in Rhode Island and are U.S. citizens or eligible non-citizens
Once approved, the child becomes Medicaid-eligible, unlocking access to:
Home Health Nursing
Personal Care Assistance (PCA)
Durable Medical Equipment (DME)
Physical, Occupational, and Speech Therapy
Assistive Technology and Behavioral Health Services
Case Management and Respite Care
3. PROVIDER SERVICES UNDER TEFRA
Approved Medicaid providers can deliver the following services to TEFRA-eligible children:
Skilled Nursing: In-home care for medically fragile children
Therapies: PT, OT, ST with age-appropriate, goal-based plans
Home-Based Behavioral Services: ABA therapy or behavioral supports
Care Coordination: Integration with school services and specialists
Equipment and Supplies: Wheelchairs, adaptive seating, communication aids
Transportation: Non-medical and medical rides to waiver-authorized services
4. ENROLLMENT & APPROVAL PROCESS (FOR FAMILIES)
Step 1: Family contacts EOHHS or accesses the online Katie Beckett application.
Step 2: Submit documentation including medical records, SSI evaluations, and financial statements (for the child only).
Step 3: A clinical review team evaluates the child’s medical needs and functional limitations.
Step 4: If approved, the child receives full Medicaid coverage through the Katie Beckett pathway.
Step 5: A case manager may be assigned to coordinate HCBS and manage the plan of care.
5. DOCUMENTATION REQUIRED (FOR PROVIDERS WORKING WITH TEFRA CLIENTS)
Provider Medicaid enrollment confirmation
NPI and licensure for clinical/therapy staff
Service Authorization from Medicaid or care coordinator
Plan of Care aligned with medical necessity and HCBS standards
Daily service notes, treatment goals, and family engagement logs
HIPAA documentation and consent forms
6. STAFFING REQUIREMENTS FOR PROVIDERS
Depending on services rendered, providers may need:
Role: RN or LPN
Requirements: Rhode Island licensure, experience with pediatric and home-based care
Role: Speech/OT/PT Therapist
Requirements: RI license, Medicaid credentialed, child-focused treatment planning
Role: Behavioral Health Provider or ABA Technician
Requirements: Credentialed in behavior analysis, experience with neurodiverse youth
Role: Care Coordinator or Case Manager
Requirements: Knowledge of Medicaid, IEPs, and wraparound supports
Training:
Pediatric safety and abuse prevention
Communication with families and guardians
Person-centered planning
Documentation and billing protocols
7. FUNDING & SERVICE DELIVERY FRAMEWORK
TEFRA-based services are funded under Rhode Island’s Medicaid State Plan. Services must meet:
Medical Necessity criteria
Least Restrictive Environment preference (home/community over institutions)
Provider Scope of Practice and Licensure rules
HCBS Settings Rule for community integration
8. TIMELINE FOR PROVIDER ENGAGEMENT
Phase: Medicaid Enrollment and Credentialing
Timeline: 30–90 days
Phase: Service Authorization and Care Planning
Timeline: Begins immediately after child approval
Phase: Service Delivery and Documentation
Ongoing: Real-time notes, quarterly reports, and Medicaid billing
9. CONTACT INFORMATION
Rhode Island Executive Office of Health and Human Services (EOHHS)
Katie Beckett Program Info: https://eohhs.ri.gov
Rhode Island Medicaid Provider Portal
Website: https://www.riproviderportal.org
Katie Beckett Parent Guide and Application
Direct Link: https://eohhs.ri.gov/katie-beckett
Centers for Medicare & Medicaid Services (CMS)
Website: https://www.cms.gov
WAIVER CONSULTING GROUP’S START-UP ASSISTANCE SERVICE — RHODE ISLAND TEFRA SERVICE PROVIDERS
WCG equips providers to support TEFRA/Katie Beckett families with quality, Medicaid-approved pediatric services.
Scope of Work:
Provider enrollment and credentialing with Medicaid
Pediatric-focused Policy & Procedure Manual development
Staff training and licensure tracking
Plan of Care templates, family communication logs, and service note formats
Compliance assistance with HCBS rules and state audits
Katie Beckett referral coordination guidance

Case Management
CASE MANAGEMENT SERVICES PROVIDER IN RHODE ISLAND
COORDINATING INDIVIDUALIZED CARE PLANS, SUPPORTS, AND RESOURCES TO PROMOTE HOLISTIC WELL-BEING AND INDEPENDENT LIVING
Case Management Services in Rhode Island are Medicaid-funded supports that help individuals navigate health, behavioral, and social service systems. These services are crucial to ensuring that people with disabilities, chronic illnesses, or aging-related needs receive person-centered care aligned with their goals. Case management is authorized under the 1115 Global Waiver, BHDDH DD Waivers, Katie Beckett/TEFRA, and Medicaid State Plan services.
1. GOVERNING AGENCIES
Agency: Rhode Island Executive Office of Health and Human Services (EOHHS)
Role: Manages Medicaid funding, provider enrollment, and service delivery standards.
Agency: Department of Behavioral Healthcare, Developmental Disabilities & Hospitals (BHDDH)
Role: Approves and monitors case managers serving individuals with developmental disabilities.
Agency: Rhode Island Department of Health (RIDOH)**
Role: May regulate case managers working in medical or clinical roles (e.g., RN case managers).
Agency: Centers for Medicare & Medicaid Services (CMS)**
Role: Defines federal requirements for case management under Medicaid HCBS waivers.
2. CASE MANAGEMENT SERVICES OVERVIEW
Case managers help individuals access services, build care teams, and coordinate supports that align with the participant’s goals. Services are person-centered and span across medical, behavioral, housing, education, and employment domains.
Approved providers may deliver:
Assessment & Planning: Conducting person-centered assessments and developing Individualized Service Plans (ISPs).
Referral Coordination: Linking participants to medical, mental health, housing, employment, and community supports.
Care Monitoring: Ensuring services are delivered as planned, and modifying ISPs as needs evolve.
Service Authorization: Submitting documentation to Medicaid or waiver programs for approval.
Crisis & Risk Management: Identifying red flags and facilitating emergency supports.
Documentation: Case notes, visit logs, quarterly progress reviews, and incident reports.
3. LICENSING & PROVIDER APPROVAL REQUIREMENTS
Prerequisites:
Register your business with the RI Secretary of State.
Obtain EIN and Type 2 NPI.
Enroll as a Medicaid Case Management Provider through the EOHHS portal.
For DD waiver case managers, apply and qualify through BHDDH.
Employ or contract qualified case managers with relevant licensure or experience.
Develop a Case Management Services Policy & Procedure Manual addressing planning, compliance, and documentation.
4. RHODE ISLAND PROVIDER ENROLLMENT PROCESS
Step 1: Form your business entity and obtain EIN/NPI.
Step 2: Apply through EOHHS to become a Medicaid case management provider.
Step 3: If serving the IDD population, submit a provider application to BHDDH.
Step 4: Submit staff qualifications, service models, and sample care plans.
Step 5: Begin receiving referrals and authorizations for case management services.
5. REQUIRED DOCUMENTATION
Business registration and Articles of Incorporation
Medicaid provider enrollment and BHDDH approval (if applicable)
NPI confirmation and insurance coverage
Staff licenses (if applicable) and background checks
Case Management Services Policy & Procedure Manual including:
Person-centered planning procedures
ISP development templates
Referral coordination workflows
Risk management and incident response protocols
Documentation and Medicaid billing templates
HIPAA compliance and participant rights documentation
6. STAFFING REQUIREMENTS
Role: Case Manager
Requirements: Degree in human services, social work, or nursing; experience with person-centered planning and system navigation.
Role: RN Case Manager (optional, if serving complex medical needs)
Requirements: Active RN license in RI, knowledge of Medicaid systems.
Role: Case Management Supervisor / Program Director
Requirements: Oversight of ISPs, staff compliance, and quality assurance processes.
All staff must complete:
Person-centered planning and HCBS Settings Rule training
HIPAA and documentation standards
Abuse prevention and crisis de-escalation
Cultural competence and disability rights
Annual reviews and continuing education (as required)
7. MEDICAID WAIVER PROGRAMS
Case Management Services are authorized through:
1115 Global Waiver (HCBS): For individuals with chronic or long-term support needs
BHDDH DD Waivers: Intensive case management for adults with intellectual/developmental disabilities
Katie Beckett/TEFRA: Case coordination for medically fragile children
Medicaid State Plan: For select medical case management services (e.g., hospital discharges, disease management)
8. TIMELINE TO LAUNCH
Phase: Business Formation & Policy Manual Creation
Timeline: 1–2 months
Phase: Medicaid and BHDDH Enrollment (if applicable)
Timeline: 2–3 months
Phase: Staff Hiring & Training
Timeline: 30–60 days
Phase: Participant Assignment & ISP Development
Timeline: Begins once case management authorizations are approved
9. CONTACT INFORMATION
Rhode Island Executive Office of Health and Human Services (EOHHS)
Website: https://eohhs.ri.gov
Department of Behavioral Healthcare, Developmental Disabilities & Hospitals (BHDDH)
Website: https://bhddh.ri.gov
Rhode Island Medicaid Provider Portal
Website: https://www.riproviderportal.org
Rhode Island Department of Health (RIDOH)
Website: https://health.ri.gov
Centers for Medicare & Medicaid Services (CMS)
Website: https://www.cms.gov
WAIVER CONSULTING GROUP’S START-UP ASSISTANCE SERVICE — RHODE ISLAND CASE MANAGEMENT PROVIDER
WCG helps launch and optimize case management services that ensure participants receive person-centered, coordinated care across the lifespan.
Scope of Work:
Medicaid and BHDDH enrollment support
ISP templates and person-centered planning guides
Referral tracking systems and coordination logs
Compliance tools for incident tracking and service monitoring
Policy & Procedure Manual tailored to case management standards
Quality assurance forms and participant satisfaction tools

Non-Medical Transportation
NON-MEDICAL TRANSPORTATION SERVICES PROVIDER IN RHODE ISLAND
PROMOTING ACCESS TO COMMUNITY LIFE, SERVICES, AND INDEPENDENCE THROUGH RELIABLE, DOOR-TO-DOOR TRANSPORTATION SUPPORT
Non-Medical Transportation (NMT) Services in Rhode Island are Medicaid-funded supports designed to help individuals with disabilities, older adults, and waiver participants access essential services, day programs, and community resources. Unlike Non-Emergency Medical Transportation (NEMT), NMT is aimed at improving community integration, independence, and participation in activities outside of health care. These services are reimbursable under Rhode Island’s 1115 Medicaid Waiver, Long-Term Services and Supports (LTSS), and Developmental Disabilities (DD) Waivers.
1. GOVERNING AGENCIES
Agency: Rhode Island Executive Office of Health and Human Services (EOHHS)
Role: Oversees Medicaid waiver programs and NMT service authorizations.
Agency: Department of Behavioral Healthcare, Developmental Disabilities & Hospitals (BHDDH)
Role: Authorizes transportation services under DD Waivers and monitors usage.
Agency: Centers for Medicare & Medicaid Services (CMS)**
Role: Provides federal oversight of HCBS programs including NMT services.
Agency: Rhode Island Public Utilities Commission (RIPUC)
Role: Regulates commercial transportation providers and ensures compliance with public safety laws (when applicable).
2. NON-MEDICAL TRANSPORTATION SERVICES OVERVIEW
NMT services support Medicaid participants in reaching community-based destinations that promote independence, employment, and social participation.
Approved providers may deliver:
Door-to-Door Transportation: To and from adult day centers, employment sites, recreational activities, and essential errands.
Fixed Route & Scheduled Services: Regular transport to vocational programs or waiver-approved services.
Escort Services (if authorized): Companion assistance during transport for safety or communication needs.
Accessible Vehicle Transport: Wheelchair lift-equipped vans and vehicles for individuals with mobility impairments.
Trip Logging & Documentation: Mileage, duration, purpose, and participant tracking for billing and audits.
3. LICENSING & PROVIDER APPROVAL REQUIREMENTS
Prerequisites:
Register your transportation business with the Rhode Island Secretary of State.
Obtain an EIN and Type 2 NPI.
Register as a Medicaid provider through the Rhode Island EOHHS portal under NMT service codes.
Obtain commercial vehicle insurance and RIPUC transportation operating authority (if transporting the general public or charging fares).
Ensure ADA-compliant vehicles if transporting individuals with physical disabilities.
Develop a Non-Medical Transportation Services Policy & Procedure Manual with safety protocols and trip documentation standards.
4. RHODE ISLAND PROVIDER ENROLLMENT PROCESS
Step 1: Register your business, secure EIN/NPI, and purchase vehicle and liability insurance.
Step 2: Apply for Medicaid provider enrollment through the RI provider portal for NMT billing codes.
Step 3: If transporting individuals in the community, apply for commercial licensing through RIPUC (as required).
Step 4: Submit vehicle safety documents, staff driver credentials, and your operating manual.
Step 5: Contract with BHDDH or Medicaid MCOs to begin receiving service referrals.
5. REQUIRED DOCUMENTATION
Articles of Incorporation and state business registration
EIN and NPI confirmation
Medicaid provider enrollment acceptance
Commercial vehicle insurance and driver liability coverage
RIPUC operating authority (if required)
Non-Medical Transportation Policy & Procedure Manual including:
Trip documentation templates and driver logs
Emergency preparedness and incident response plans
Participant intake, rights, and consent forms
Safety training and vehicle maintenance schedules
ADA compliance, lift operation, and securement protocols
Medicaid billing and audit documentation forms
6. STAFFING REQUIREMENTS
Role: Transportation Driver / Escort
Requirements: Clean driving record, background check, CPR/First Aid (preferred), defensive driving course, and disability sensitivity training.
Role: Dispatcher / Scheduler
Requirements: Coordinates daily trips, manages routing software, and ensures timely pickups and drop-offs.
All staff must complete:
HIPAA and confidentiality training
Vehicle safety, lift usage, and emergency evacuation procedures
Abuse prevention and safe transport practices
Documentation and Medicaid billing training
Annual driving record checks and in-service refreshers
7. MEDICAID WAIVER PROGRAMS
Non-Medical Transportation is authorized through:
Global Consumer Choice Compact 1115 Waiver (RI Medicaid): Supports NMT as part of community integration services.
BHDDH DD Waivers (e.g., Community Living, Shared Living): Covers transport to day programs, jobs, and supported activities.
Self-Directed Waiver Services: Allows participants to arrange transportation using approved providers.
LTSS-Managed Care MCOs: May contract directly with NMT vendors for integrated support services.
8. TIMELINE TO LAUNCH
Phase: Business Formation & Manual Development
Timeline: 1–2 months
Phase: Medicaid Enrollment & RIPUC Authorization
Timeline: 2–3 months
Phase: Vehicle Acquisition, Driver Hiring & Training
Timeline: 30–60 days
Phase: Referral Activation & Service Initiation
Timeline: Begins once authorization and scheduling agreements are in place
9. CONTACT INFORMATION
Rhode Island Executive Office of Health and Human Services (EOHHS)
Website: https://eohhs.ri.gov
Rhode Island Medicaid Provider Portal
Website: https://www.riproviderportal.org
Department of Behavioral Healthcare, Developmental Disabilities & Hospitals (BHDDH)
Website: https://bhddh.ri.gov
Rhode Island Public Utilities Commission (RIPUC) – Transportation Licensing
Website: https://ripuc.ri.gov
Centers for Medicare & Medicaid Services (CMS)
Website: https://www.cms.gov
WAIVER CONSULTING GROUP’S START-UP ASSISTANCE SERVICE — RHODE ISLAND NON-MEDICAL TRANSPORTATION PROVIDER
WCG assists transportation providers in launching Medicaid-compliant operations that expand access and mobility for Rhode Island’s waiver populations.
Scope of Work:
Business registration, Medicaid enrollment, and RIPUC guidance
Custom Policy & Procedure Manual for NMT operations
Driver credentialing and safety training checklists
Vehicle compliance logs, lift safety protocols, and rider intake forms
Medicaid trip log templates and EVV-compatible records
Contracts with BHDDH and managed care referral partners
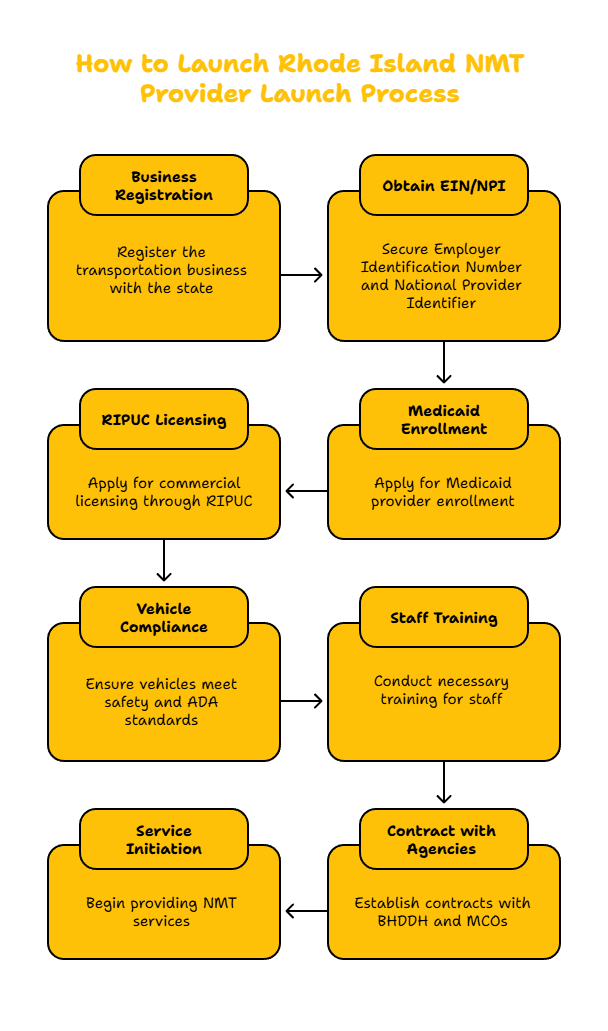
Home Health
HOME HEALTH CARE SERVICES PROVIDER IN RHODE ISLAND
DELIVERING SKILLED NURSING, THERAPIES, AND SUPPORTIVE IN-HOME CARE TO IMPROVE HEALTH AND INDEPENDENCE ACROSS RHODE ISLAND COMMUNITIES
Home Health Care Services in Rhode Island are Medicaid-covered medical and supportive services provided in an individual’s home by licensed professionals. These services are essential for individuals recovering from illness, managing chronic conditions, or requiring long-term skilled care. Home health care is administered under Rhode Island Medicaid, the State Plan, and waiver programs, with oversight from the Rhode Island Department of Health (RIDOH) and the Executive Office of Health and Human Services (EOHHS).
1. GOVERNING AGENCIES
Agency: Rhode Island Executive Office of Health and Human Services (EOHHS)
Role: Administers Medicaid and LTSS benefits, including home health authorizations.
Agency: Rhode Island Department of Health (RIDOH)
Role: Licenses and inspects Home Nursing Care Providers and Home Care Providers.
Agency: Centers for Medicare & Medicaid Services (CMS)**
Role: Establishes federal compliance standards for Medicaid-funded home health agencies.
Agency: Community HealthChoices Managed Care Organizations (CHC MCOs)
Role: Authorize and reimburse home health services under integrated care models.
2. HOME HEALTH CARE SERVICES OVERVIEW
These services allow medically eligible individuals to receive necessary nursing and therapy in the comfort of their home, preventing institutionalization and promoting recovery.
Approved providers may deliver:
Skilled Nursing Services: Medication administration, wound care, disease management, and monitoring.
Home Health Aide Services: Basic care such as bathing, dressing, feeding, and mobility assistance.
Physical, Occupational, and Speech Therapy: Post-hospital rehab and long-term functional support.
Medical Social Work: Case management, counseling, and community resource navigation.
Telehealth (if authorized): Remote monitoring and virtual visits to supplement care.
Care Coordination & Documentation: Plan of care development, physician updates, and Medicaid billing compliance.
3. LICENSING & PROVIDER APPROVAL REQUIREMENTS
Prerequisites:
Register your agency with the Rhode Island Secretary of State.
Obtain an EIN and Type 2 NPI.
Apply for licensure as a Home Nursing Care Provider (for skilled services) or Home Care Provider (for aide services) through RIDOH.
Enroll in Rhode Island Medicaid and PROMISe™ as a home health provider.
Maintain professional liability and workers’ compensation insurance.
Develop a Home Health Care Services Policy & Procedure Manual following RIDOH and Medicaid guidelines.
4. RHODE ISLAND PROVIDER ENROLLMENT PROCESS
Step 1: Form your legal entity and obtain EIN, NPI, and required insurance policies.
Step 2: Submit a licensure application to RIDOH for either home nursing or home care services.
Step 3: Enroll in the Medicaid provider network via the RI provider portal.
Step 4: Contract with Medicaid MCOs and submit required staffing, policy, and readiness documentation.
Step 5: Once approved, receive service authorizations and begin accepting clients.
5. REQUIRED DOCUMENTATION
Articles of Incorporation and business registration
EIN and NPI verification
RIDOH license as Home Nursing or Home Care Provider
Insurance certificates (liability, malpractice, workers’ comp)
Home Health Care Policy & Procedure Manual including:
Clinical care protocols and RN supervisory procedures
HIPAA compliance and participant consent policies
Emergency response, medication handling, and infection control
Shift notes, electronic visit verification (EVV), and billing logs
Admission assessment forms and discharge planning checklists
6. STAFFING REQUIREMENTS
Role: Registered Nurse (RN)
Requirements: RI nursing license; responsible for assessments, care plans, and staff supervision.
Role: Licensed Practical Nurse (LPN)
Requirements: Licensed by RIDOH; assists with clinical tasks under RN direction.
Role: Home Health Aide (HHA)
Requirements: Completion of certified training program; background checks; CPR/First Aid.
Role: Physical, Occupational, or Speech Therapist
Requirements: RI licensure in respective discipline; physician referral required.
Role: Program Administrator
Requirements: Manages operations, scheduling, compliance, and clinical staff coordination.
All staff must complete:
Orientation and skills competency validation
HIPAA and patient rights training
Infection control and emergency preparedness education
Documentation and billing compliance protocols
7. MEDICAID WAIVER PROGRAMS
Home Health Care Services are available under:
Rhode Island Medicaid State Plan: Covers physician-referred skilled care and aide support.
Global Consumer Choice Compact 1115 Waiver: Allows broader HCBS access including home nursing.
BHDDH DD Waivers: May authorize home health for individuals with developmental disabilities.
Katie Beckett Program: Supports skilled in-home care for medically complex children.
8. TIMELINE TO LAUNCH
Phase: Business Registration & Policy Manual Creation
Timeline: 1–2 months
Phase: RIDOH Licensure & Medicaid Enrollment
Timeline: 2–3 months
Phase: Staff Hiring, Credentialing & Compliance Training
Timeline: 30–60 days
Phase: Contracting & Service Launch
Timeline: Begins upon approval and authorization
9. CONTACT INFORMATION
Rhode Island Executive Office of Health and Human Services (EOHHS)
Website: https://eohhs.ri.gov
Rhode Island Medicaid Provider Portal
Website: https://www.riproviderportal.org
Rhode Island Department of Health – Home Care Licensure
Website: https://health.ri.gov/licenses/detail.php?id=282
Centers for Medicare & Medicaid Services (CMS)
Website: https://www.cms.gov
WAIVER CONSULTING GROUP’S START-UP ASSISTANCE SERVICE — RHODE ISLAND HOME HEALTH CARE PROVIDER
WCG helps new and expanding agencies launch fully licensed and compliant home health services tailored to Rhode Island’s Medicaid and managed care systems.
Scope of Work:
Business registration, RIDOH licensing, and Medicaid enrollment
Custom Home Health Care Policy & Procedure Manual
Staff credentialing checklists and compliance logs
EVV setup and visit note documentation templates
Intake forms, care plan templates, and clinical supervision tools
Contracting guidance with Medicaid MCOs and billing assistance

Meal & Nutrition
MEAL & NUTRITION SERVICES PROVIDER IN RHODE ISLAND
DELIVERING NUTRITIOUS MEALS AND DIETARY SUPPORT TO PROMOTE HEALTH, INDEPENDENCE, AND QUALITY OF LIFE FOR INDIVIDUALS WITH DISABILITIES AND AGING NEEDS
Meal & Nutrition Services in Rhode Island help individuals maintain their health through access to balanced, medically appropriate meals and nutritional education. These supports are funded through Rhode Island Medicaid, including the 1115 Global Waiver, State Plan, and various Home and Community-Based Services (HCBS) Waiver programs. Services are designed to support individuals at risk of malnutrition, poor health outcomes, or who are unable to prepare meals independently.
1. GOVERNING AGENCIES
Agency: Rhode Island Executive Office of Health and Human Services (EOHHS)
Role: Oversees Medicaid service authorizations, provider enrollment, and reimbursement for home-delivered meals and nutrition supports.
Agency: Department of Behavioral Healthcare, Developmental Disabilities & Hospitals (BHDDH)
Role: Coordinates nutrition support for waiver participants with intellectual/developmental disabilities (IDD).
Agency: Rhode Island Department of Health (RIDOH)**
Role: Regulates food safety and sanitation for meal preparation, particularly for licensed kitchens and food service facilities.
Agency: Centers for Medicare & Medicaid Services (CMS)**
Role: Defines federal criteria for HCBS nutrition services under Medicaid waivers.
2. MEAL & NUTRITION SERVICES OVERVIEW
These services are aimed at individuals with functional limitations, dietary restrictions, or medical conditions requiring tailored meal preparation and delivery.
Approved providers may deliver:
Home-Delivered Meals: Ready-to-eat, refrigerated, or frozen meals tailored to participant needs (e.g., low-sodium, diabetic, texture-modified).
Congregate Meal Services (optional): Group meals in licensed adult day or community centers.
Nutrition Counseling: Assessment and guidance from a Registered Dietitian (RD) for medically complex individuals.
Feeding Assistance: In-home help with safe eating and monitoring nutritional intake.
Menu Planning: Specialized menus based on ISP or physician directives.
Documentation: Meal delivery logs, dietary assessments, and nutrition tracking.
3. LICENSING & PROVIDER APPROVAL REQUIREMENTS
Prerequisites:
Register your business with the RI Secretary of State.
Obtain EIN and Type 2 NPI.
Enroll with EOHHS as a Medicaid provider of home-delivered or congregate meals.
Meet RIDOH food service safety requirements and obtain food establishment licensure (if preparing meals).
Partner with a licensed commercial kitchen or caterer, if not operating your own facility.
Develop a Meal & Nutrition Services Policy & Procedure Manual detailing meal prep, delivery, dietary protocols, and documentation standards.
4. RHODE ISLAND PROVIDER ENROLLMENT PROCESS
Step 1: Register your business entity and secure EIN/NPI.
Step 2: Obtain food preparation license (if applicable) or contract with a licensed vendor.
Step 3: Enroll as a Medicaid provider for meal/nutritional support under waiver categories.
Step 4: Submit staff qualifications (e.g., RDs), kitchen licenses, and sample menus.
Step 5: Begin meal service upon service authorization.
5. REQUIRED DOCUMENTATION
Business registration, EIN, and NPI confirmation
Medicaid provider enrollment approval
RIDOH food safety certificate or kitchen partnership documentation
Insurance coverage (liability, workers’ comp, product liability)
Meal & Nutrition Services Policy & Procedure Manual including:
Food handling and delivery protocols
Menu planning and customization procedures
Documentation and meal delivery tracking forms
Nutrition counseling templates and assessment tools
HIPAA compliance, participant rights, and incident reporting protocols
Quality assurance and feedback collection methods
6. STAFFING REQUIREMENTS
Role: Meal Program Coordinator
Requirements: Experience in food service or case management; oversees scheduling and dietary compliance.
Role: Delivery Personnel
Requirements: Background check, food handling training, and transportation license.
Role (optional): Registered Dietitian (RD)
Requirements: Licensed in RI, provides nutritional assessments and counseling.
All staff must complete:
Food safety and sanitation training
HIPAA and confidentiality compliance
Abuse prevention and dignity-in-care training
Emergency response for in-home meal services
Annual skills evaluations (if assisting with feeding)
7. MEDICAID WAIVER PROGRAMS
Meal & Nutrition Services are reimbursable under:
1115 Global Waiver (HCBS): For individuals requiring nutritional support to remain at home
BHDDH DD Waivers: For adults with IDD needing special diets or meal planning
Katie Beckett/TEFRA Program: For children with medically necessary dietary needs
State Plan Services (Limited): May cover nutrition counseling with RD referral
Self-Directed Waivers: Participants may choose vendors for meal preparation and delivery
8. TIMELINE TO LAUNCH
Phase: Business Registration & Policy Manual Development
Timeline: 1–2 months
Phase: RIDOH Food License & Medicaid Enrollment
Timeline: 1–2 months
Phase: Staff Hiring, Kitchen Setup & Delivery Logistics
Timeline: 30–60 days
Phase: Participant Assignment & Menu Customization
Timeline: Begins once referrals and authorizations are received
9. CONTACT INFORMATION
Rhode Island Executive Office of Health and Human Services (EOHHS)
Website: https://eohhs.ri.gov
Department of Behavioral Healthcare, Developmental Disabilities & Hospitals (BHDDH)
Website: https://bhddh.ri.gov
Rhode Island Department of Health (RIDOH)
Food Safety: https://health.ri.gov/food
Rhode Island Medicaid Provider Portal
Website: https://www.riproviderportal.org
Centers for Medicare & Medicaid Services (CMS)
Website: https://www.cms.gov
WAIVER CONSULTING GROUP’S START-UP ASSISTANCE SERVICE — RHODE ISLAND MEAL & NUTRITION SERVICES PROVIDER
WCG helps launch compliant, person-centered nutrition services that meet Medicaid guidelines and participant needs.
Scope of Work:
Medicaid enrollment and RIDOH food safety licensure guidance
Policy & Procedure Manual tailored to meal prep and delivery
Meal log templates and dietary assessment tools
Staff onboarding tools and food safety checklists
Menu planning forms and participant feedback systems

Our Client Portal offers a wealth of resources that you can explore related to various programs and state requirements.